Prostate cancer
| Prostate cancer | |
|---|---|
| Synonyms | Carcinoma of the prostate |
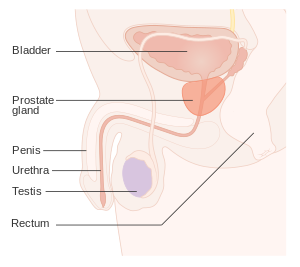 | |
| Position of the prostate | |
| Specialty | Oncology, urology |
| Symptoms | None, difficulty urinating, blood in the urine, pain in the pelvis, back, or when urinating[1][2] |
| Usual onset | Age > 50[3] |
| Risk factors | Older age, family history, race[3] |
| Diagnostic method | Tissue biopsy, medical imaging[2] |
| Differential diagnosis | Benign prostatic hyperplasia[1] |
| Treatment | Active surveillance, surgery, radiation therapy, hormone therapy, chemotherapy[2] |
| Prognosis | 5-year survival rate 99% (US)[4] |
| Frequency | 1.1 million new cases (2014)[5] |
| Deaths | 307,000 (2014)[5] |
Prostate cancer is the development of cancer in the prostate, a gland in the male reproductive system.[6] Most prostate cancers are slow growing; however, some grow relatively quickly.[1][3] The cancer cells may spread from the prostate to other areas of the body, particularly the bones and lymph nodes.[7] It may initially cause no symptoms.[1] In later stages, it can lead to difficulty urinating, blood in the urine or pain in the pelvis, back, or when urinating.[2] A disease known as benign prostatic hyperplasia may produce similar symptoms.[1] Other late symptoms may include feeling tired due to low levels of red blood cells.[1]
Factors that increase the risk of prostate cancer include older age, a family history of the disease, and race.[3] About 99% of cases occur in males over the age of 50.[3] Having a first-degree relative with the disease increases the risk two to threefold.[3] In the United States, it is more common in the African American population than the White American population.[3] Other factors that may be involved include a diet high in processed meat, red meat or milk products or low in certain vegetables.[3] An association with gonorrhea has been found, but a reason for this relationship has not been identified.[8] An increased risk is associated with the BRCA mutations.[9] Prostate cancer is diagnosed by biopsy.[2]Medical imaging may then be done to determine if the cancer has spread to other parts of the body.[2]
Prostate cancer screening is controversial.[3][10]Prostate-specific antigen (PSA) testing increases cancer detection, but it is controversial regarding whether it improves outcomes.[10][11][12] Informed decision making is recommended when it comes to screening among those 55 to 69 years old.[13][14] Testing, if carried out, is more reasonable in those with a longer life expectancy.[15] While 5α-reductase inhibitors appear to decrease low-grade cancer risk, they do not affect high-grade cancer risk and thus are not recommended for prevention.[3] Supplementation with vitamins or minerals does not appear to affect the risk.[3][16]
Many cases are managed with active surveillance or watchful waiting.[2] Other treatments may include a combination of surgery, radiation therapy, hormone therapy or chemotherapy.[2] When it only occurs inside the prostate, it may be curable.[1] In those in whom the disease has spread to the bones, pain medications, bisphosphonates and targeted therapy, among others, may be useful.[2] Outcomes depend on a person's age and other health problems as well as how aggressive and extensive the cancer is.[2] Most men with prostate cancer do not end up dying from the disease.[2] The 5-year survival rate in the United States is 99%.[4] Globally, it is the second most common type of cancer and the fifth leading cause of cancer-related death in men.[5] In 2012, it occurred in 1.1 million men and caused 307,000 deaths.[5] It was the most common cancer in males in 84 countries,[3] occurring more commonly in the developed world.[17] Rates have been increasing in the developing world.[17] Detection increased significantly in the 1980s and 1990s in many areas due to increased PSA testing.[3] Studies of males who died from unrelated causes have found prostate cancer in 30% to 70% of those over age 60.[1]
.mw-parser-output .toclimit-2 .toclevel-1 ul,.mw-parser-output .toclimit-3 .toclevel-2 ul,.mw-parser-output .toclimit-4 .toclevel-3 ul,.mw-parser-output .toclimit-5 .toclevel-4 ul,.mw-parser-output .toclimit-6 .toclevel-5 ul,.mw-parser-output .toclimit-7 .toclevel-6 uldisplay:none
Contents
1 Signs and symptoms
2 Risk factors
2.1 Genetics
2.2 Dietary
2.3 Medication exposure
2.4 Infection
2.5 Environmental
2.6 Sexual
3 Pathophysiology
4 Diagnosis
4.1 Prostate imaging
4.2 Biopsy
4.2.1 Gleason score
4.3 Tumor markers
4.4 Staging
5 Prevention
5.1 Diet and lifestyle
5.2 Medications
6 Screening
7 Management
7.1 Surveillance
7.2 Aggressive cancer
7.3 Castration-resistant
7.4 Palliative care
8 Prognosis
8.1 Classification systems
8.2 Life expectancy
9 Epidemiology
9.1 United States
9.2 Canada
9.3 Europe
10 History
11 Society and culture
12 Research
12.1 CRPC
12.2 Pre-clinical
12.3 Cancer models
12.4 Infections
12.5 Diagnosis
13 See also
14 References
15 External links
Signs and symptoms
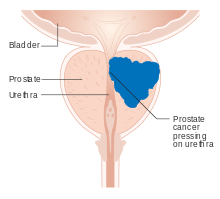
A diagram of prostate cancer pressing on the urethra, which can cause symptoms.
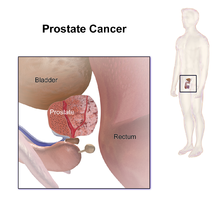
Prostate cancer
Early prostate cancer usually has no clear symptoms. Sometimes prostate cancer does cause symptoms, often similar to those of diseases such as benign prostatic hyperplasia. These include frequent urination, nocturia (increased urination at night), difficulty starting and maintaining a steady stream of urine, hematuria (blood in the urine), and dysuria (painful urination). A study based on the 1998 Patient Care Evaluation in the US found that about a third of patients diagnosed with prostate cancer had one or more such symptoms, while two-thirds had no symptoms.[18]
Prostate cancer is associated with urinary dysfunction as the prostate gland surrounds the prostatic urethra. Changes within the gland, therefore, directly affect urinary function. Because the vas deferens deposits seminal fluid into the prostatic urethra, and secretions from the prostate gland itself are included in semen content, prostate cancer may also cause problems with sexual function and performance, such as difficulty achieving erection or painful ejaculation.[18]
Metastatic prostate cancer that has spread to other parts of the body can cause additional symptoms. The most common symptom is bone pain, often in the vertebrae (bones of the spine), pelvis, or ribs. Spread of cancer into other bones such as the femur is usually to the proximal or nearby part of the bone. Prostate cancer in the spine can also compress the spinal cord, causing tingling, leg weakness and urinary and fecal incontinence.[19]
Risk factors
A complete understanding of the causes of prostate cancer remains elusive.[20] The primary risk factors are obesity, age, and family history. Prostate cancer is very uncommon in men younger than 45, but becomes more common with advancing age. The average age at the time of diagnosis is 70.[21] Many men never know they have prostate cancer. Autopsy studies of Chinese, German, Israeli, Jamaican, Swedish, and Ugandan men who died of other causes have found prostate cancer in 30% of men in their fifties, and in 80% of men in their seventies.[22]
Men who have first-degree family members with prostate cancer appear to have double the risk of getting the disease compared to men without prostate cancer in the family.[23] This risk appears to be greater for men with an affected brother than for men with an affected father. In the United States in 2005, there were an estimated 230,000 new cases of prostate cancer and 30,000 deaths due to prostate cancer.[24] Men with high blood pressure are more likely to develop prostate cancer.[25] There is a small increased risk of prostate cancer associated with lack of exercise.[26]
Genetics
Genetic background may contribute to prostate cancer risk, as suggested by associations with race, family, and specific gene variants. Men who have a first-degree relative (father or brother) with prostate cancer have twice the risk of developing prostate cancer, and those with two first-degree relatives affected have a fivefold greater risk compared with men with no family history.[27] In the United States, prostate cancer more commonly affects black men than white or Hispanic men, and is also more deadly in black men.[28][29] In contrast, the incidence and mortality rates for Hispanic men are one third lower than for non-Hispanic whites. Studies of twins in Scandinavia suggest that 40% of prostate cancer risk can be explained by inherited factors.[30]
No single gene is responsible for prostate cancer; many different genes have been implicated. Mutations in BRCA1 and BRCA2, important risk factors for ovarian cancer and breast cancer in women, have also been implicated in prostate cancer.[31] Other linked genes include the Hereditary Prostate cancer gene 1 (HPC1), the androgen receptor, and the vitamin D receptor.[28]TMPRSS2-ETS gene family fusion, specifically TMPRSS2-ERG or TMPRSS2-ETV1/4 promotes cancer cell growth.[32] These fusions can arise via complex rearrangement chains called chromoplexy.[33]
Two large genome-wide association studies linking single-nucleotide polymorphisms (SNPs) to prostate cancer were published in 2008.[34][35] These studies identified several SNPs which substantially affect the risk of prostate cancer. For example, individuals with TT allele pair at SNP rs10993994 were reported to be at 1.6 times higher risk of prostate cancer than those with the CC allele pair. This SNP explains part of the increased prostate cancer risk of African American men as compared to American men of European descent, since the C allele is much more prevalent in the latter; this SNP is located in the promoter region of the MSMB gene, thus affects the amount of MSMB protein synthesized and secreted by epithelial cells of the prostate.[36]
Finally, obesity[37] and elevated blood levels of testosterone[38] may increase the risk for prostate cancer.
Dietary
Consuming fruits and vegetables has been found to be of little benefit in preventing prostate cancer.[39] Evidence supports little role for dietary fruits and vegetables in prostate cancer occurrence.[40] Red meat and processed meat also appear to have little effect in human studies.[41] Higher meat consumption has been associated with a higher risk in some studies.[42]
Lower blood levels of vitamin D may increase the risk of developing prostate cancer.[43]
Folic acid supplements have no effect on the risk of developing prostate cancer.[44]
Medication exposure
There are also some links between prostate cancer and medications, medical procedures, and medical conditions.[45] Use of the cholesterol-lowering medications known as statins may also decrease prostate cancer risk.[46]
Infection
Infection or inflammation of the prostate (prostatitis) may increase the chance for prostate cancer while another study shows infection may help prevent prostate cancer by increasing blood flow to the area. In particular, infection with the sexually transmitted infections chlamydia, gonorrhea, or syphilis seems to increase risk.[8][47]
Papilloma virus has been proposed in several studies to have a potential role in prostate cancer, but as of 2015 the evidence was inconclusive.[48] A review in 2018 suggested there may be an increased risk but noted that this increased risk was still debatable.[49]
Environmental
Research released in May 2007 found that US war veterans who had been exposed to Agent Orange had a 48% increased risk of prostate cancer recurrence following surgery.[50]
Sexual
Although there is some evidence from prospective cohort studies that frequent ejaculation may reduce prostate cancer risk,[51] there are no results from randomized controlled trials concluding that this benefit exists.[52] There is an association between vasectomy and prostate cancer, but more research is needed to determine if this is a causal relationship.[53]
Pathophysiology

The prostate is a part of the male reproductive system that helps make and store seminal fluid. In adult men, a typical prostate is about 3 centimeters long and weighs about 20 grams.[54] It is located in the pelvis, under the urinary bladder and in front of the rectum. The prostate surrounds part of the urethra, the tube that carries urine from the bladder during urination and semen during ejaculation.[55] Because of its location, prostate diseases often affect urination, ejaculation, and rarely defecation. The prostate contains many small glands which make about 20% of the fluid constituting semen.[56]
In prostate cancer, the cells of these prostate glands mutate into cancer cells. The prostate glands require male hormones, known as androgens, to work properly. Androgens include testosterone, which is made in the testes; dehydroepiandrosterone, made in the adrenal glands; and dihydrotestosterone, which is converted from testosterone within the prostate itself. Androgens are also responsible for secondary sex characteristics such as facial hair and increased muscle mass.

Prostate cancer that has metastasized to the lymph nodes

Prostate cancer that has metastasized to the bone
Most prostate cancers are classified as adenocarcinomas, or glandular cancers, that begin when normal semen-secreting prostate gland cells mutate into cancer cells. The region of prostate gland where the adenocarcinoma is most common is the peripheral zone. Initially, small clumps of cancer cells remain confined to otherwise normal prostate glands, a condition known as carcinoma in situ or prostatic intraepithelial neoplasia (PIN). Although there is no proof that PIN is a cancer precursor, it is closely associated with cancer. Over time, these cancer cells begin to multiply and spread to the surrounding prostate tissue (the stroma) forming a tumor.
Eventually, the tumor may grow large enough to invade nearby organs such as the seminal vesicles or the rectum, or the tumor cells may develop the ability to travel in the bloodstream and lymphatic system. Prostate cancer is considered a malignant tumor because it is a mass of cells that can invade other areas of the body. This invasion of other organs is called metastasis. Prostate cancer most commonly metastasizes to the bones, lymph nodes, and may invade rectum, bladder and lower ureters after local progression. The route of metastasis to bone is thought to be venous as the prostatic venous plexus draining the prostate connects with the vertebral veins.[57]
The prostate is a zinc-accumulating, citrate-producing organ. The protein ZIP1 is responsible for the active transport of zinc into prostate cells. One of the zinc's important roles is to change the metabolism of the cell in order to produce citrate, an important component of semen. The process of zinc accumulation, alteration of metabolism, and citrate production is energy inefficient, and prostate cells sacrifice enormous amounts of energy (ATP) in order to accomplish this task. Prostate cancer cells are generally devoid of zinc. This allows prostate cancer cells to save energy not making citrate, and utilize the new abundance of energy to grow and spread. The absence of zinc is thought to occur via a silencing of the gene that produces the transporter protein ZIP1. ZIP1 is now called a tumor suppressor gene product for the gene SLC39A1. The cause of the epigenetic silencing is unknown. Strategies which transport zinc into transformed prostate cells effectively eliminate these cells in animals. Zinc inhibits NF-κB pathways, is anti-proliferative and induces apoptosis in abnormal cells. Unfortunately, oral ingestion of zinc is ineffective since high concentrations of zinc into prostate cells is not possible without the active transporter, ZIP1.[58]
Loss of cancer suppressor genes, early in the prostatic carcinogenesis, have been localized to chromosomes 8p, 10q, 13q, and 16q. P53 mutations in the primary prostate cancer are relatively low and are more frequently seen in metastatic settings, hence, p53 mutations are a late event in the pathology of prostate cancer. Other tumor suppressor genes that are thought to play a role in prostate cancer include PTEN (gene) and KAI1. "Up to 70 percent of men with prostate cancer have lost one copy of the PTEN gene at the time of diagnosis"[59]
Relative frequency of loss of E-cadherin and CD44 has also been observed.
RUNX2 is a transcription factor that prevents cancer cells from undergoing apoptosis thereby contributing to the development of prostate cancer.[60]
The PI3k/Akt signaling cascade works with the transforming growth factor beta/SMAD signaling cascade to ensure prostate cancer cell survival and protection against apoptosis.[61] X-linked inhibitor of apoptosis (XIAP) is hypothesized to promote prostate cancer cell survival and growth and is a target of research because if this inhibitor can be shut down then the apoptosis cascade can carry on its function in preventing cancer cell proliferation.[62]Macrophage inhibitory cytokine-1 (MIC-1) stimulates the focal adhesion kinase (FAK) signaling pathway which leads to prostate cancer cell growth and survival.[63]
The androgen receptor helps prostate cancer cells to survive and is a target for many anti cancer research studies; so far, inhibiting the androgen receptor has only proven to be effective in mouse studies.[64]
Prostate specific membrane antigen (PSMA) stimulates the development of prostate cancer by increasing folate levels for the cancer cells to use to survive and grow; PSMA increases available folates for use by hydrolyzing glutamated folates.[65]
Diagnosis

If already having grown large, a prostate cancer may first be detected on CT scan.
The American Cancer Society's position regarding early detection by PSA testing is "Research has not yet proven that the potential benefits of testing outweigh the harms of testing and treatment. The American Cancer Society believes that men should not be tested without learning about what we know and don’t know about the risks and possible benefits of testing and treatment. Starting at age 50, (45 if African American or brother or father suffered from condition before age 65) talk to your doctor about the pros and cons of testing so you can decide if testing is the right choice for you."[66]
There are also several other tests that can be used to gather more information about the prostate and the urinary tract. Digital rectal examination (DRE) may allow a doctor to detect prostate abnormalities. Cystoscopy shows the urinary tract from inside the bladder, using a thin, flexible camera tube inserted down the urethra. Transrectal ultrasonography creates a picture of the prostate using sound waves from a probe in the rectum. But the only test that can fully confirm the diagnosis of prostate cancer is a biopsy, the removal of small pieces of the prostate for microscopic examination.
Prostate imaging
Ultrasound (US) and magnetic resonance imaging (MRI) are the two main imaging methods used for prostate cancer detection. Urologists use transrectal ultrasound during prostate biopsy and can sometimes see a hypoechoic area (tissues or structures that reflect relatively less of the ultrasound waves directed at them). As ultrasound has poor tissue resolution, it is generally not used clinically.
Prostate MRI has better soft tissue resolution than ultrasound.[67]
MRI in those who are at low risk might help people choose active surveillance, in those who are at intermediate risk it may help with determining the stage of disease, while in those who are at high risk it might help find bone disease.[68]
Currently (2011), MRI is used to identify targets for prostate biopsy using fusion MRI with ultrasound (US) or MRI-guidance alone. In men who are candidates for active surveillance, fusion MR/US guided prostate biopsy detected 33% of cancers compared to 7% with standard ultrasound guided biopsy.[69]
Prostate MRI is also used for surgical planning for men undergoing robotic prostatectomy. It has also shown to help surgeons decide whether to resect or spare the neurovascular bundle, determine return to urinary continence, and help assess surgical difficulty.[70]
For Prostate MRI exists the PI-RADS Reporting system. PI-RADS is an acronym for Prostate Imaging-Reporting and Data System, defining standards of high-quality clinical service for multi-parametric Magnetic Resonance Imaging (mpMRI), including image creation and reporting.
Biopsy

Prostate needle biopsy

Micrograph showing a prostate cancer (conventional adenocarcinoma) with perineural invasion. H&E stain.
If cancer is suspected, a biopsy is offered expediently. During a biopsy a urologist or radiologist obtains tissue samples from the prostate via the rectum. A biopsy gun inserts and removes special hollow-core needles (usually three to six on each side of the prostate) in less than a second. Prostate biopsies are routinely done on an outpatient basis and rarely require hospitalization. Antibiotics should be used to prevent complications like fever, urinary tract infections, and sepsis[71] even if the most appropriate course or dose of the antibiotic is still undefined.[72] Fifty-five percent of men report discomfort during prostate biopsy.[73]
Gleason score
The tissue samples are then examined under a microscope to determine whether cancer cells are present, and to evaluate the microscopic features (or Gleason score) of any cancer found. Prostate specific membrane antigen is a transmembrane carboxypeptidase and exhibits folate hydrolase activity.[74] This protein is overexpressed in prostate cancer tissues and is associated with a higher Gleason score.[74]
Tumor markers
Tissue samples can be stained for the presence of PSA and other tumor markers in order to determine the origin of malignant cells that have metastasized.[75]
Small cell carcinoma is a very rare (1%[76]) type of prostate cancer that cannot be diagnosed using the PSA.[76][77] As of 2009[update] researchers were investigating ways to screen for this type of prostate cancer, because it is quick to spread to other parts of the body.[77]
The oncoprotein BCL-2 is associated with the development of androgen-independent prostate cancer, due to its high levels of expression in androgen-independent tumours in advanced stages of the pathology. The upregulation of BCL-2 after androgen ablation in prostate carcinoma cell lines and in a castrated-male rat model further established a connection between BCL-2 expression and prostate cancer progression.[78]
The expression of Ki-67 by immunohistochemistry may be a significant predictor of patient outcome for men with prostate cancer.[79]
Staging

Diagram showing T1-3 stages of prostate cancer.
An important part of evaluating prostate cancer is determining the stage, or how far the cancer has spread. Knowing the stage helps define prognosis and is useful when selecting therapies. The most common system is the four-stage TNM system (abbreviated from Tumor/Nodes/Metastases). Its components include the size of the tumor, the number of involved lymph nodes, and the presence of any other metastases.[80]
The most important distinction made by any staging system is whether or not the cancer is still confined to the prostate. In the TNM system, clinical T1 and T2 cancers are found only in the prostate, while T3 and T4 cancers have spread elsewhere. Several tests can be used to look for evidence of spread. Medical specialty professional organizations recommend against the use of PET scans, CT scans, or bone scans when a physician stages early prostate cancer with low risk for metastasis.[81] Those tests would be appropriate in such cases as when a CT scan evaluates spread within the pelvis, a bone scan look for spread to the bones, and endorectal coil magnetic resonance imaging to closely evaluate the prostatic capsule and the seminal vesicles. Bone scans should reveal osteoblastic appearance due to increased bone density in the areas of bone metastasis—opposite to what is found in many other cancers that metastasize.
After a prostate biopsy, a pathologist looks at the samples under a microscope. If cancer is present, the pathologist reports the grade of the tumor. The grade tells how much the tumor tissue differs from normal prostate tissue and suggests how fast the tumor is likely to grow. The Gleason system is used to grade prostate tumors from 2 to 10, where a Gleason score of 10 indicates the most abnormalities. The pathologist assigns a number from 1 to 5 for the most common pattern observed under the microscope, then does the same for the second-most-common pattern. The sum of these two numbers is the Gleason score. The Whitmore-Jewett stage is another method sometimes used.

Sclerosis of the bones of the thoracic spine due to prostate cancer metastases (CT image)
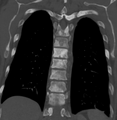
Sclerosis of the bones of the thoracic spine due to prostate cancer metastases (CT image)

Sclerosis of the bones of the pelvis due to prostate cancer metastases
Prevention
Diet and lifestyle
The data on the relationship between diet and prostate cancer is poor.[82] In light of this the rate of prostate cancer is linked to the consumption of the Western diet.[82] There is little if any evidence to support an association between trans fat, saturated fat, and carbohydrate intake and risk of prostate cancer.[82][83] Evidence regarding the role of omega-3 fatty acids in preventing prostate cancer does not suggest that they reduce the risk of prostate cancer, although additional research is needed.[82][84] Vitamin supplements appear to have no effect and some may increase the risk.[16][82] High calcium intake has been linked to advanced prostate cancer.[85]
Consuming fish may lower prostate cancer deaths but does not appear to affect its occurrence.[86] Some evidence supports lower rates of prostate cancer with a vegetarian diet.[87] There is some tentative evidence for foods containing lycopene and selenium.[88][89] Diets rich in cruciferous vegetables, soy, beans and other legumes may be associated with a lower risk of prostate cancer, especially more advanced cancers.[90]
Men who get regular exercise may have a slightly lower risk, especially vigorous activity and the risk of advanced prostate cancer.[90]
Medications
In those who are being regularly screened, 5-alpha-reductase inhibitors (finasteride and dutasteride) reduce the overall risk of being diagnosed with prostate cancer, but there are insufficient data to determine if they have an effect on the risk of death and they may increase the chance of more serious cases.[91]
Screening
Prostate cancer screening is an effort to find unsuspected cancers in those without symptoms. Options include the digital rectal exam (DRE) and the prostate-specific antigen (PSA) blood test.[92] Such screening is controversial[93] and, for many, may lead to unnecessary disruption and possibly harmful consequences.[94] Harms of population-based screening, primarily due to over-diagnosis (the detection of latent cancers which would have otherwise gone symptomless and undiscovered) may outweigh the benefits.[92] Others recommend shared decision-making; an approach where individual have the option to undergo screening after thorough consultation with their physician about the positives and negatives.[95]
The United States Preventive Services Task Force (USPSTF) suggests the decision whether or not to have PSA screening be based on decision making between the patient and physician for men 55 to 69 years of age.[11] USPSTF recommends against PSA screening for males who are age 70 or older.[13] The Centers for Disease Control and Prevention shared USPSTF's prior conclusion.[96] The American Society of Clinical Oncology and the American College of Physicians discourage screening for those who are expected to live less than ten to fifteen years, while in those with a greater life expectancy a decision should be made by the person in question based on the potential risks and benefits.[97] In general, they concluded, "it is uncertain whether the benefits associated with PSA testing for prostate cancer screening are worth the harms associated with screening and subsequent unnecessary treatment."[98]
American Urological Association (AUA 2013) guidelines call for weighing the benefits of preventing prostate cancer mortality in 1 man for every 1,000 men screened over a ten-year period against the known harms associated with diagnostic tests and treatment. The AUA recommends offering screening to those 55 to 69 be based on shared decision making, and that if screening is performed it should occur no more often than every two years.[99] In the United Kingdom as of 2015 there is no program to screen for prostate cancer.[12]
Management
The first decision to be made in managing prostate cancer is whether treatment is needed. Prostate cancer, especially low-grade forms found in elderly men, often grows so slowly that no treatment is required.[100] Treatment may also be inappropriate if a person has other serious health problems or is not expected to live long enough for symptoms to appear. Alternative approaches that delay active treatment and instead involve surveillance of diagnosed prostate cancers are termed expectant management.[100] Expectant management is divided into two approaches: Watchful Waiting, which has palliative intent, and Active Surveillance, which has curative intent.[100]
Which option is best depends on the stage of the disease, the Gleason score, and the PSA level. Other important factors are age, general health, and a person's views about potential treatments and their possible side effects. Because most treatments can have significant side effects, such as erectile dysfunction and urinary incontinence, treatment discussions often focus on balancing the goals of therapy with the risks of lifestyle alterations. A combination of the treatment options is often recommended for managing prostate cancer.[101][102][103]
Guidelines for treatment for specific clinical situations requires a good estimation of a person's long-term life expectancy.[104] People can also use an 18-item questionnaire to learn whether they have good knowledge and understanding about their treatment options before they choose. Most of those who are newly diagnosed and made a treatment choice can not correctly answer over half of the questions.[104] Radiotherapy and surgery appear to result in similar outcomes with respect to bowel, erectile and urinary function after five years.[105]
If radiation therapy is done first, and fails, then radical prostatectomy may be an option though it becomes a very technically challenging surgery, is associated with decreased quality of life and may not be feasible.[106] On the other hand, radiation therapy done after surgical failure may have many complications.[107] It is associated with a small increase in bladder and colon cancer.[108]
In localized disease, it is unknown if radical prostatectomy is better or worse than watchful waiting.[109]
A meta-analysis on the effects of voiding position during urination in males with prostate enlargement showed that sitting was superior to standing. Bladder emptying was significantly improved, while there was a trend towards a higher urinary flow and shorter voiding time.[110]
Surveillance
Many men diagnosed with low-risk prostate cancer are eligible for active surveillance. This means that careful observation of the tumor is conducted over time, with the intention of initiating treatment if there are signs of cancer progression. Active surveillance is not synonymous with watchful waiting, an older term which implies no treatment or specific program of monitoring, with the assumption that palliative, not curative, treatment would be used if advanced, symptomatic disease develops.[100]
Active surveillance involves monitoring the tumor for signs of growth or the appearance of symptoms. The monitoring process may involve serial PSA tests, physical examination of the prostate, and/or repeated biopsies. The goal of surveillance is to avoid overtreatment and the sometimes serious, permanent side effects of treatment for a slow-growing or self-limited tumor (that in most people, would be unlikely to cause problems). This approach is not used for aggressive cancers, but it may cause anxiety for people who wrongly believe that all cancer is deadly or themselves to have life-threatening cancer. For 50% to 75% of people with prostate cancer it will cause no harm before a person dies from other causes.[111]
Aggressive cancer
Treatment of metastatic prostate cancer can be difficult.[112] Treatment of aggressive prostate cancers may involve surgery (i.e. radical prostatectomy), radiation therapy including brachytherapy (prostate brachytherapy), external beam radiation therapy, high-intensity focused ultrasound (HIFU), chemotherapy, oral chemotherapeutic drugs (temozolomide/TMZ), cryosurgery, hormonal therapy, or some combination.[113][114]
Although the widespread use of prostate-specific antigen (PSA) screening in the US has resulted in diagnosis at earlier age and cancer stage, the vast majority of cases are still diagnosed in men older than 65 years, and approximately 25% of cases are diagnosed in men older than 75 years.[115] Though US National Comprehensive Cancer Network guidelines recommend using life expectancy greater than or less than 10 years to help make treatment decisions, in practice, many elderly patients are not offered curative treatment options such as radical prostatectomy or radiation therapy and are instead treated with hormonal therapy or watchful waiting.[116] This pattern can be attributed to factors such as medical co-morbidity and patient preferences is regard to quality of life in addition to prostate cancer specific risk factors such as pretreatment PSA, Gleason score and clinical stage. As the average life expectancy increases due to advances in the treatment of cardiovascular, pulmonary and other chronic diseases, it is likely that more elderly patients will be living long enough to suffer the consequences of their prostate cancer. Therefore, there is currently much interest in the role of aggressive prostate cancer treatment modalities such as with surgery or radiation in the elderly population who have localized disease.
If the cancer has spread beyond the prostate, treatment options significantly change, so most doctors that treat prostate cancer use a variety of nomograms to predict the probability of spread. Treatment by watchful waiting/active surveillance, external beam radiation therapy, brachytherapy, cryosurgery, HIFU, and surgery are, in general, offered to men whose cancer remains within the prostate. Hormonal therapy and chemotherapy are often reserved for disease that has spread beyond the prostate. There are exceptions: local or metastasis-directed therapy by radiation treatment may be used for advanced tumors with a limited amount of metastases,[117] and hormonal therapy is used for some early stage tumors. Cryotherapy (the process of freezing the tumor), hormonal therapy, and chemotherapy may also be offered if initial treatment fails and the cancer progresses.
Sipuleucel-T, a cancer vaccine has been found to result in a benefit (a four-month increase in survival) for men with metastatic prostate cancer.[118]
Castration-resistant
Most hormone dependent cancers become resistant to treatment after one to three years and resume growth despite hormone therapy. Previously considered "hormone-refractory prostate cancer" or "androgen-independent prostate cancer", the term castration-resistant has replaced "hormone refractory" because while they are no longer responsive to castration treatment (reduction of available androgen/testosterone/DHT by chemical or surgical means), these cancers still show reliance upon hormones for androgen receptor activation.[119]
The cancer chemotherapic docetaxel has been used as treatment for CRPC with a median survival benefit of 2 to 3 months.[120][121] A second-line chemotherapy treatment is cabazitaxel.[122] A combination of bevacizumab, docetaxel, thalidomide and prednisone appears effective in the treatment of CRPC.[123]
The immunotherapy treatment with sipuleucel-T in CRPC increases survival by 4 months.[124] The second line hormonal therapy abiraterone increases survival by 4.6 months when compared to placebo.[125]Enzalutamide is another second line hormonal agent with a 5-month survival advantage over placebo. Both abiraterone and enzalutamide are currently being tested in clinical trials in those with CRPC who have not previously received chemotherapy.[126][127]
Only a subset of people respond to androgen signaling blocking drugs and certain cells with characteristics resembling stem cells remain unaffected.[128][129] Therefore, the desire to improve outcome of people with CRPC has resulted in the claims of increasing doses further or combination therapy with synergistic androgen signaling blocking agents.[130] But even these combination will not affect stem-like cells that do not exhibit androgen signaling. It is possible that for further advances, a combination of androgen signaling blocking agent with stem-like cell directed differentiation therapy drug would prove ideal.[131]
Palliative care
Treatment of metastatic prostate cancer can be difficult.[112] Treatment of aggressive prostate cancers may involve surgery (i.e. radical prostatectomy), radiation therapy including brachytherapy (prostate brachytherapy), external beam radiation therapy, high-intensity focused ultrasound (HIFU), chemotherapy, oral chemotherapeutic drugs (temozolomide/TMZ), cryosurgery, hormonal therapy, or some combination.[113][114]
Prognosis
Prostate cancer rates are higher in developed countries than in the rest of the world. Many of the risk factors for prostate cancer are more common in developed countries, including longer life expectancy and diets higher in red meat. Also, where there is greater access to screening programs, there is a higher detection rate.
In the United States, prostate cancer that is local or regional at the time of diagnosis has a 5-year survival rate of nearly 100%, while those with distant metastases have a 5-year survival rate of 29%.[132] In Japan, death from prostate cancer was one-fifth to one-half the rates in the United States and Europe in the 1990s.[133] In India in the 1990s, half of the people with prostate cancer confined to the prostate died within 19 years.[134] African-American men have 50–60 times more prostate cancer and prostate cancer deaths than men in Shanghai, China.[135] In Nigeria, 2% of men develop prostate cancer, and 64% of them are dead after 2 years.[136] Most Nigerian men present with metastatic disease with a typical survival of 40 months.[137]
In patients who undergo treatment, the most important clinical prognostic indicators of disease outcome are the stage, pretherapy PSA level, and Gleason score. In general, the higher the grade and the stage, the poorer the prognosis. Nomograms can be used to calculate the estimated risk of the individual patient. The predictions are based on the experience of large groups of patients suffering from cancers at various stages.[138]
In 1941, Charles Huggins reported that androgen ablation therapy causes regression of primary and metastatic androgen-dependent prostate cancer.[139] He was awarded the 1966 Nobel Prize for Physiology or Medicine for this discovery. Androgen ablation therapy causes remission in 80-90% of patients undergoing therapy, resulting in a median progression-free survival of 12 to 33 months. After remission, an androgen-independent phenotype typically emerges, wherein the median overall survival is 23–37 months from the time of initiation of androgen ablation therapy.[140] It is not clear how the prostate cancer becomes androgen-independent or how it reestablishes progression, although a few possibilities (on how) have been proposed.[141] And the way the cancer changes, to overcome the lack of androgen, may vary between individual patients.
Classification systems

Micrograph of prostate adenocarcinoma, acinar type, the most common type of prostate cancer. Needle biopsy, H&E stain
Many prostate cancers are not destined to be lethal, and most men will ultimately not die as a result of the disease. Decisions about treatment type and timing may, therefore, be informed by an estimation of the risk that the tumor will ultimately recur after treatment and/or progress to metastases and mortality. Several tools are available to help predict outcomes, such as pathologic stage and recurrence after surgery or radiation therapy. Most combine stage, grade, and PSA level, and some also add the number or percentage of biopsy cores positive, age, and/or other information.
- The D'Amico classification stratifies men by low, intermediate, or high risk based on stage, grade, and PSA. It is used widely in clinical practice and research settings. The major downside to the 3-level system is that it does not account for multiple adverse parameters (e.g., high Gleason score and high PSA) in stratifying patients.
- The Partin tables[142] predict pathologic outcomes (margin status, extraprostatic extension, and seminal vesicle invasion) based on the same three variables and are published as lookup tables.
- The Kattan nomograms predict recurrence after surgery and/or radiation therapy, based on data available either at the time of diagnosis or after surgery. The nomograms can be calculated using paper graphs or software available on a website or for handheld computers. The Kattan score represents the likelihood of remaining free of disease at a given time interval following treatment.
- The UCSF Cancer of the Prostate Risk Assessment (CAPRA) score predicts both pathologic status and recurrence after surgery. It offers comparable accuracy as the Kattan preoperative nomogram and can be calculated without paper tables or a calculator. Points are assigned based on PSA, Grade, stage, age, and percentage of cores positive; the sum yields a 0–10 score, with every 2 points representing roughly a doubling of risk of recurrence. The CAPRA score was derived from community-based data in the CaPSURE database. It has been validated among over 10,000 prostatectomy patients, including patients from CaPSURE;[143] the SEARCH registry, representing data from several Veterans Administration and active military medical centers;[144] a multi-institutional cohort in Germany;[145] and the prostatectomy cohort at Johns Hopkins University.[146] More recently, it has been shown to predict metastasis and mortality following prostatectomy, radiation therapy, watchful waiting, or androgen deprivation therapy.[147]
Life expectancy
Life expectancy projections are averages for an entire male population, and many medical and lifestyle factors modify these numbers. For example, studies have shown that a 40-year-old man will lose 3.1 years of life if he is overweight (BMI 25-29) and 5.8 years of life if he is obese (BMI 30 or more), compared to men of normal weight. If he is both overweight and a smoker, he will lose 6.7 years, and if obese and a smoker, he will lose 13.7 years.[148]
At this time, there is no evidence that either surgery or beam radiation has an advantage over the other in this regard, the lower death rates reported with surgery appear to occur because surgery is more likely to be offered to younger men with less serious forms of cancer. Insufficient information is available to determine whether seed radiation extends life more readily than the other treatments, but data so far do not suggest that it does.[149]
People with low-grade disease (Gleason 2-4) were unlikely to die of prostate cancer within 15 years of diagnosis. Older men (age 70-75) with low-grade disease had an approximately 20% overall survival at 15 years due to deaths from competing causes. Men with high-grade disease (Gleason 8-10) experienced high prostate cancer mortality within 15 years of diagnosis, regardless of their age at diagnosis, underscoring the very aggressive nature of poorly differentiated prostate cancer.[150]
Epidemiology

Age-standardized death from prostate cancer per 100,000 inhabitants in 2004.[151].mw-parser-output .refbeginfont-size:90%;margin-bottom:0.5em.mw-parser-output .refbegin-hanging-indents>ullist-style-type:none;margin-left:0.mw-parser-output .refbegin-hanging-indents>ul>li,.mw-parser-output .refbegin-hanging-indents>dl>ddmargin-left:0;padding-left:3.2em;text-indent:-3.2em;list-style:none.mw-parser-output .refbegin-100font-size:100%
no data
<4
4-8
8-12
12-16
16-20
20-24
24-28
28-32
32-36
36-40
40-44
>44
As of 2012, prostate cancer is the second most frequently diagnosed cancer (at 15% of all male cancers)[152] and the sixth leading cause of cancer death in males worldwide.[153] In 2010, prostate cancer resulted in 256,000 deaths, up from 156,000 deaths in 1990.[154] Rates of prostate cancer vary widely across the world. Although the rates vary widely between countries, it is least common in South and East Asia, and more common in Europe, North America, Australia, and New Zealand.[155] Prostate cancer is least common among Asian men and most common among black men, with figures for white men in between.[156][157]
The average annual incidence rate of prostate cancer between 1988 and 1992 among Chinese men in the United States was 15 times higher than that of their counterparts living in Shanghai and Tianjin,[156][157][158] but these high rates may be affected by increasing rates of detection.[159] Many suggest that prostate cancer may be under-reported, yet BPH incidence in China and Japan is similar to rates in Western countries.[160][161]
More than 80% of men will develop prostate cancer by the age of 80.[162] In the majority of cases, cancer will be slow-growing and of little concern. In such men, diagnosing prostate cancer is overdiagnosis—the needless identification of a technically aberrant condition that will never harm the patient—and treatment in such men exposes them to all of its adverse effects, with no possibility of extending their lives.[163]
United States

New cases and deaths from prostate cancer in the United States per 100,000 males between 1975 and 2014
It is estimated that in 2018, approximately 164,690 new cases and 29,430 prostate cancer–related deaths will occur in the United States. Prostate cancer is now the second leading cause of cancer death in men, exceeded by lung cancer and colorectal cancer. It accounts for 19% of all male cancers and 9% of male cancer-related deaths. Age-adjusted incidence rates increased steadily from 1975 through 1992, with particularly dramatic increases associated with the inception of widespread use of prostate-specific antigen (PSA) screening in the late 1980s and early 1990s, followed by a fall in incidence. A decline in early-stage prostate cancer incidence rates from 2011 to 2012 (19%) in men aged 50 years and older persisted through 2013 (6%).
Between 2013 and 2015, mortality rates appear to have stabilized. It has been suggested that declines in mortality rates in certain jurisdictions reflect the benefit of PSA screening,[3] but others have noted that these observations may be explained by independent phenomena such as improved treatments. The estimated lifetime risk of a prostate cancer diagnosis is about 14.0%, and the lifetime risk of dying from this disease is 2.6%. Cancer statistics from the American Cancer Society and the National Cancer Institute (NCI) indicated that between 2005 and 2011, the proportion of disease diagnosed at a locoregional stage was 93% for whites and 92% for African Americans; the proportion of disease diagnosed at a late stage was 4% for whites and 5% for African Americans. An autopsy study of white and Asian men also found an increase in occult prostate cancer with age, reaching nearly 60% in men older than 80 years. More than 50% of cancers in Asian men and 25% of cancers in white men had a Gleason score of 7 or greater, suggesting that Gleason score may be an imprecise indicator of clinically insignificant prostate cancer.[164]
Canada
Prostate cancer is the third leading cause of cancer in Canadian men. In 2016, around 4,000 died and 21,600 men were diagnosed with prostate cancer.[93]
Europe
In Europe in 2012 it was the 3rd most diagnosed cancer after breast and colorectal at 417,000 cases.[165]
In the United Kingdom it is also the second most common cause of cancer death after lung cancer, where around 35,000 cases are diagnosed every year and of which around 10,000 die of it.[166]
History
Although the prostate was first described by Venetian anatomist Niccolò Massa in 1536, and illustrated by Flemish anatomist Andreas Vesalius in 1538, prostate cancer was not identified until 1853.[167] Prostate cancer was initially considered a rare disease, probably because of shorter life expectancies and poorer detection methods in the 19th century. The first treatments of prostate cancer were surgeries to relieve urinary obstruction.[168] Removal of the entire gland (radical perineal prostatectomy) was first performed in 1904 by Hugh H. Young at Johns Hopkins Hospital.[169] Surgical removal of the testes (orchiectomy) to treat prostate cancer was first performed in the 1890s, but with limited success. Transurethral resection of the prostate (TURP) replaced radical prostatectomy for symptomatic relief of obstruction in the middle of the 20th century because it could better preserve penile erectile function. Radical retropubic prostatectomy was developed in 1983 by Patrick Walsh.[170] This surgical approach allowed for removal of the prostate and lymph nodes with maintenance of penile function.
In 1941, Charles B. Huggins published studies in which he used estrogen to oppose testosterone production in men with metastatic prostate cancer. This discovery of "chemical castration" won Huggins the 1966 Nobel Prize in Physiology or Medicine.[171] The role of the gonadotropin-releasing hormone (GnRH) in reproduction was determined by Andrzej W. Schally and Roger Guillemin, who both won the 1977 Nobel Prize in Physiology or Medicine for this work. GnRH receptor agonists, such as leuprorelin and goserelin, were subsequently developed and used to treat prostate cancer.[172][173]
Radiation therapy for prostate cancer was first developed in the early 20th century and initially consisted of intraprostatic radium implants. External beam radiotherapy became more popular as stronger [X-ray] radiation sources became available in the middle of the 20th century. Brachytherapy with implanted seeds (for prostate cancer) was first described in 1983.[174]
Systemic chemotherapy for prostate cancer was first studied in the 1970s. The initial regimen of cyclophosphamide and 5-fluorouracil was quickly joined by multiple regimens using a host of other systemic chemotherapy drugs.[175]
Society and culture
People with prostate cancer generally encounter significant disparities in awareness, funding, media coverage, and research—and therefore, inferior treatment and poorer outcomes—compared to other cancers of equal prevalence.[176] In 2001, The Guardian noted that Britain had 3,000 nurses specializing in breast cancer, compared to only one for prostate cancer. It also discovered that the waiting time between referral and diagnosis was two weeks for breast cancer but three months for prostate cancer.[177] A 2007 report by the U.S.-based National Prostate Cancer Coalition stated that for every prostate cancer drug on the market, there were seven used to treat breast cancer. The Times also noted an "anti-male bias in cancer funding" with a four-to-one discrepancy in the United Kingdom by both the government and by cancer charities such as Cancer Research UK.[176][178] Equality campaigners such as author Warren Farrell cite such stark spending inequalities as a clear example of governments unfairly favouring women's health over men's health.[179]
Disparities also extend into areas such as detection, with governments failing to fund or mandate prostate cancer screening while fully supporting breast cancer programs. For example, a 2007 report found 49 U.S. states mandate insurance coverage for routine breast cancer screening, compared to 28 for prostate cancer.[180] Prostate cancer also experiences significantly less media coverage than other, equally prevalent cancers, with a study by Prostate Coalition showing 2.6 breast cancer stories for each one covering cancer of the prostate.[176]
Prostate Cancer Awareness Month takes place in September in a number of countries. A light blue ribbon is used to promote the cause.[181][182]
Research
CRPC
MDV3100 was in phase III trials for CRPC (chemo-naive and post-chemo patient populations)[183] and gained FDA approval in 2012 as enzalutamide for the treatment of castration-resistant prostate cancer.[126][127]
Alpharadin completed a phase 3 trial for CRPC patients with bone metastasis. A pre-planned interim analysis showed improved survival and quality of life. The study was stopped for ethical reasons to give the placebo group the same treatment. Alpharadin uses bone targeted Radium-223 isotopes to kill cancer cells by alpha radiation.[184][unreliable medical source?] It was approved by the U.S. Food and Drug Administration (FDA) on May, 15th 2013 ahead of schedule under the priority review program.[185] Alpharadin still waits for approval by the European Medicines Agency (EMA).
As of 2016[update]PARP inhibitor olaparib has shown promise in clinical trials for CRPC.[186] Also in trials for CRPC are : checkpoint inhibitor ipilimumab, CYP17 inhibitor galeterone (TOK-001), and immunotherapy PROSTVAC.[186]
All medications for CRPC block AR signaling via direct or indirect targeting of the AR ligand binding domain (LBD). Over the last decade molecules that could successfully target these alternative domains have emerged.[187] Such therapies could provide an advantage; particularly in treating prostate cancers that are resistant to current therapies like enzalutamide.[187]
Pre-clinical
Arachidonate 5-lipoxygenase has been identified as playing a significant role in the survival of prostate cancer cells.[188][189][190] Medications which target this enzyme may be an effective therapy for limiting tumor growth and cancer metastasis as well as inducing programmed cell death in cancer cells.[188][189][190] In particular, arachidonate 5-lipoxygenase inhibitors produce massive, rapid programmed cell death in prostate cancer cells.[188][189][190]
Several medications that target alternative domains on the androgen receptor (DNA binding domain - DBD, and transactivation domain - TAD) or degrade cellular AR protein have reached clinical trials, while some are in pre-clinical development.[187] These therapies hold promis in treating AR dependent prostate cancers both in early and late stage, because many have shown the ability to target both the full-length and the splice-variant forms of the androgen receptor.[187]
Cancer models
Scientists have established a few prostate cancer cell lines to investigate the mechanism involved in the progression of prostate cancer. LNCaP, PC-3 (PC3), and DU-145 (DU145) are commonly used prostate cancer cell lines. The LNCaP cancer cell line was established from a human lymph node metastatic lesion of prostatic adenocarcinoma. PC-3 and DU-145 cells were established from human prostatic adenocarcinoma metastatic to bone and to brain, respectively. LNCaP cells express androgen receptor (AR), but PC-3 and DU-145 cells express very little or no AR. AR, an androgen-activated transcription factor, belongs to the steroid nuclear receptor family. Development of the prostate is dependent on androgen signaling mediated through AR, and AR is also important during the development of prostate cancer.
The proliferation of LNCaP cells is androgen-dependent but the proliferation of PC-3 and DU-145 cells is androgen-insensitive. Elevation of AR expression is often observed in advanced prostate tumors in patients.[191][192] Some androgen-independent LNCaP sublines have been developed from the ATCC androgen-dependent LNCaP cells after androgen deprivation for study of prostate cancer progression. These androgen-independent LNCaP cells have elevated AR expression and express prostate specific antigen upon androgen treatment. The paradox is that androgens inhibit the proliferation of these androgen-independent prostate cancer cells.[193][194][195]
Infections
In 2006, a previously unknown retrovirus, Xenotropic MuLV-related virus (XMRV), was associated with human prostate tumors,[196] but subsequent reports on the virus were contradictory,[197][198] and the original 2006 finding was instead due to a previously undetected contamination.[199] The journals Science and PlosONE both retracted XMRV related articles.[200][201]
Diagnosis
At present, an active area of research and non-clinically applied investigations involve non-invasive methods of prostate tumor detection. A molecular test that detects the presence of cell-associated PCA3 mRNA in fluid obtained from the prostate and first-void urine sample has also been under investigation. PCA3 mRNA is expressed almost exclusively by prostate cells and has been shown to be highly over-expressed in prostate cancer cells. The test result is currently reported as a specimen ratio of PCA3 mRNA to PSA mRNA.
Although not a replacement for serum PSA level, the PCA3 test is an additional tool to help decide whether, in men suspected of having prostate cancer (especially if an initial biopsy fails to explain the elevated serum PSA), a biopsy/rebiopsy is really needed. The higher the expression of PCA3 in the sample, the greater the likelihood of a positive biopsy; i.e., the presence of cancer cells in the prostate.[202]
See also
- Prostate Cancer Foundation
References
^ abcdefgh "Prostate Cancer Treatment (PDQ) – Health Professional Version". National Cancer Institute. 2014-04-11. Archived from the original on 5 July 2014. Retrieved 1 July 2014..mw-parser-output cite.citationfont-style:inherit.mw-parser-output .citation qquotes:"""""""'""'".mw-parser-output .citation .cs1-lock-free abackground:url("//upload.wikimedia.org/wikipedia/commons/thumb/6/65/Lock-green.svg/9px-Lock-green.svg.png")no-repeat;background-position:right .1em center.mw-parser-output .citation .cs1-lock-limited a,.mw-parser-output .citation .cs1-lock-registration abackground:url("//upload.wikimedia.org/wikipedia/commons/thumb/d/d6/Lock-gray-alt-2.svg/9px-Lock-gray-alt-2.svg.png")no-repeat;background-position:right .1em center.mw-parser-output .citation .cs1-lock-subscription abackground:url("//upload.wikimedia.org/wikipedia/commons/thumb/a/aa/Lock-red-alt-2.svg/9px-Lock-red-alt-2.svg.png")no-repeat;background-position:right .1em center.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registrationcolor:#555.mw-parser-output .cs1-subscription span,.mw-parser-output .cs1-registration spanborder-bottom:1px dotted;cursor:help.mw-parser-output .cs1-ws-icon abackground:url("//upload.wikimedia.org/wikipedia/commons/thumb/4/4c/Wikisource-logo.svg/12px-Wikisource-logo.svg.png")no-repeat;background-position:right .1em center.mw-parser-output code.cs1-codecolor:inherit;background:inherit;border:inherit;padding:inherit.mw-parser-output .cs1-hidden-errordisplay:none;font-size:100%.mw-parser-output .cs1-visible-errorfont-size:100%.mw-parser-output .cs1-maintdisplay:none;color:#33aa33;margin-left:0.3em.mw-parser-output .cs1-subscription,.mw-parser-output .cs1-registration,.mw-parser-output .cs1-formatfont-size:95%.mw-parser-output .cs1-kern-left,.mw-parser-output .cs1-kern-wl-leftpadding-left:0.2em.mw-parser-output .cs1-kern-right,.mw-parser-output .cs1-kern-wl-rightpadding-right:0.2em
^ abcdefghijk "Prostate Cancer Treatment (PDQ) – Patient Version". National Cancer Institute. 2014-04-08. Archived from the original on 5 July 2014. Retrieved 1 July 2014.
^ abcdefghijklm World Cancer Report 2014. World Health Organization. 2014. pp. Chapter 5.11. ISBN 978-9283204299.
^ ab "SEER Stat Fact Sheets: Prostate Cancer". NCI. Archived from the original on 6 July 2014. Retrieved 18 June 2014.
^ abcd World Cancer Report 2014. World Health Organization. 2014. pp. Chapter 1.1. ISBN 978-9283204299.
^ "Prostate Cancer". National Cancer Institute. January 1980. Archived from the original on 12 October 2014. Retrieved 12 October 2014.
^ Ruddon, Raymond W. (2007). Cancer biology (4th ed.). Oxford: Oxford University Press. p. 223. ISBN 9780195175431. Archived from the original on 2015-09-15.
^ ab Caini S, Gandini S, Dudas M, Bremer V, Severi E, Gherasim A (August 2014). "Sexually transmitted infections and prostate cancer risk: a systematic review and meta-analysis". Cancer Epidemiology. 38 (4): 329–38. doi:10.1016/j.canep.2014.06.002. PMID 24986642.
^ Lee MV, Katabathina VS, Bowerson ML, Mityul MI, Shetty AS, Elsayes KM, et al. (2016). "BRCA-associated Cancers: Role of Imaging in Screening, Diagnosis, and Management". Radiographics. 37 (4): 1005–1023. doi:10.1148/rg.2017160144. PMID 28548905.
^ ab "Prostate Cancer Treatment". National Cancer Institute. 6 February 2018. Retrieved 1 March 2018.Controversy exists regarding the value of screening... reported no clear evidence that screening for prostate cancer decreases the risk of death from prostate cancer
^ ab Catalona WJ (March 2018). "Prostate Cancer Screening". The Medical Clinics of North America. 102 (2): 199–214. doi:10.1016/j.mcna.2017.11.001. PMC 5935113. PMID 29406053.
^ ab "PSA testing". nhs.uk. 3 January 2015. Retrieved 5 March 2018.
^ ab "Final Recommendation Statement: Prostate Cancer: Screening - US Preventive Services Task Force". www.uspreventiveservicestaskforce.org. USPSTF. Retrieved 30 August 2018.
^ Grossman DC, Curry SJ, Owens DK, Bibbins-Domingo K, Caughey AB, Davidson KW, et al. (May 2018). "Screening for Prostate Cancer: US Preventive Services Task Force Recommendation Statement". JAMA. 319 (18): 1901–1913. doi:10.1001/jama.2018.3710. PMID 29801017.
^ Cabarkapa S, Perera M, McGrath S, Lawrentschuk N (December 2016). "Prostate cancer screening with prostate-specific antigen: A guide to the guidelines". Prostate International. 4 (4): 125–129. doi:10.1016/j.prnil.2016.09.002. PMC 5153437. PMID 27995110.
^ ab Stratton J, Godwin M (June 2011). "The effect of supplemental vitamins and minerals on the development of prostate cancer: a systematic review and meta-analysis". Family Practice. 28 (3): 243–52. doi:10.1093/fampra/cmq115. PMID 21273283.
^ ab Baade PD, Youlden DR, Krnjacki LJ (February 2009). "International epidemiology of prostate cancer: geographical distribution and secular trends". Molecular Nutrition & Food Research. 53 (2): 171–84. doi:10.1002/mnfr.200700511. PMID 19101947.
^ ab Miller DC, Hafez KS, Stewart A, Montie JE, Wei JT (September 2003). "Prostate carcinoma presentation, diagnosis, and staging: an update form the National Cancer Data Base". Cancer. 98 (6): 1169–78. doi:10.1002/cncr.11635. PMID 12973840.
^ van der Cruijsen-Koeter IW, Vis AN, Roobol MJ, Wildhagen MF, de Koning HJ, van der Kwast TH, et al. (July 2005). "Comparison of screen detected and clinically diagnosed prostate cancer in the European randomized study of screening for prostate cancer, section rotterdam". Urol. 174 (1): 121–5. doi:10.1097/01.ju.0000162061.40533.0f. PMID 15947595.
^ Hsing AW, Chokkalingam AP (2006). "Prostate cancer epidemiology". Frontiers in Bioscience. 11: 1388–413. doi:10.2741/1891. PMID 16368524.
^ Hankey BF, Feuer EJ, Clegg LX, Hayes RB, Legler JM, Prorok PC, et al. (June 16, 1999). "Cancer surveillance series: interpreting trends in prostate cancer—part I: Evidence of the effects of screening in recent prostate cancer incidence, mortality, and survival rates". J Natl Cancer Inst. 91 (12): 1017–24. doi:10.1093/jnci/91.12.1017. PMID 10379964.
^ Breslow N, Chan CW, Dhom G, Drury RA, Franks LM, Gellei B, et al. (November 15, 1977). "Latent carcinoma of prostate at autopsy in seven areas. The International Agency for Research on Cancer, Lyons, France". Int J Cancer. 20 (5): 680–8. doi:10.1002/ijc.2910200506. PMID 924691.
^ Zeegers MP, Jellema A, Ostrer H (2003). "Empiric risk of prostate carcinoma for relatives of patients with prostate carcinoma: a meta-analysis". Cancer. 97 (8): 1894–903. doi:10.1002/cncr.11262. PMID 12673715.
^ Jemal A, Murray T, Ward E, Samuels A, Tiwari RC, Ghafoor A, Feuer EJ, Thun MJ (2005). "Cancer statistics, 2005". CA Cancer J Clin. 55 (1): 10–30. doi:10.3322/canjclin.55.1.10. PMID 15661684.
^ Martin RM, Vatten L, Gunnell D, Romundstad P (March 2010). "Blood pressure and risk of prostate cancer: cohort Norway (CONOR)". Cancer Causes Control. 21 (3): 463–72. doi:10.1007/s10552-009-9477-x. PMID 19949849.
^ Friedenreich CM, Neilson HK, Lynch BM (Sep 2010). "State of the epidemiological evidence on physical activity and cancer prevention". European Journal of Cancer. 46 (14): 2593–604. doi:10.1016/j.ejca.2010.07.028. PMID 20843488.
^ Steinberg GD, Carter BS, Beaty TH, Childs B, Walsh PC (1990). "Family history and the risk of prostate cancer". Prostate. 17 (4): 337–47. doi:10.1002/pros.2990170409. PMID 2251225.
^ ab Gallagher RP, Fleshner N (October 1998). "Prostate cancer: 3. Individual risk factors" (PDF). CMAJ. 159 (7): 807–13. PMC 1232741. PMID 9805030. Archived (PDF) from the original on 2009-12-29.
^ Hoffman RM, Gilliland FD, Eley JW, Harlan LC, Stephenson RA, Stanford JL, Albertson PC, Hamilton AS, Hunt WC, Potosky AL (March 2001). "Racial and ethnic differences in advanced-stage prostate cancer: the Prostate Cancer Outcomes Study". J. Natl. Cancer Inst. 93 (5): 388–95. doi:10.1093/jnci/93.5.388. PMID 11238701.
^ Lichtenstein P, Holm NV, Verkasalo PK, Iliadou A, Kaprio J, Koskenvuo M, Pukkala E, Skytthe A, Hemminki K (July 2000). "Environmental and heritable factors in the causation of cancer--analyses of cohorts of twins from Sweden, Denmark, and Finland". N. Engl. J. Med. 343 (2): 78–85. doi:10.1056/NEJM200007133430201. PMID 10891514.
^ Struewing JP, Hartge P, Wacholder S, Baker SM, Berlin M, McAdams M, et al. (May 1997). "The risk of cancer associated with specific mutations of BRCA1 and BRCA2 among Ashkenazi Jews". The New England Journal of Medicine. 336 (20): 1401–8. doi:10.1056/NEJM199705153362001. PMID 9145676.
^ Beuzeboc P, Soulié M, Richaud P, Salomon L, Staerman F, Peyromaure M, et al. (December 2009). "[Fusion genes and prostate cancer. From discovery to prognosis and therapeutic perspectives]". Progres en Urologie (in French). 19 (11): 819–24. doi:10.1016/j.purol.2009.06.002. PMID 19945666.
^ Baca SC, Prandi D, Lawrence MS, Mosquera JM, Romanel A, Drier Y, et al. (April 2013). "Punctuated evolution of prostate cancer genomes". Cell. 153 (3): 666–77. doi:10.1016/j.cell.2013.03.021. PMC 3690918. PMID 23622249.
^ Eeles RA, Kote-Jarai Z, Giles GG, Olama AA, Guy M, Jugurnauth SK, et al. (March 2008). "Multiple newly identified loci associated with prostate cancer susceptibility". Nature Genetics. 40 (3): 316–21. doi:10.1038/ng.90. PMID 18264097.
^ Thomas G, Jacobs KB, Yeager M, Kraft P, Wacholder S, Orr N, et al. (March 2008). "Multiple loci identified in a genome-wide association study of prostate cancer". Nature Genetics. 40 (3): 310–5. doi:10.1038/ng.91. PMID 18264096.
^ Whitaker HC, Kote-Jarai Z, Ross-Adams H, Warren AY, Burge J, George A, et al. (Oct 13, 2010). Vickers A, ed. "The rs10993994 risk allele for prostate cancer results in clinically relevant changes in microseminoprotein-beta expression in tissue and urine". PLOS One. 5 (10): e13363. Bibcode:2010PLoSO...513363W. doi:10.1371/journal.pone.0013363. PMC 2954177. PMID 20967219.
^ Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ (April 2003). "Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults". N. Engl. J. Med. 348 (17): 1625–38. doi:10.1056/NEJMoa021423. PMID 12711737.
^ Gann PH, Hennekens CH, Ma J, Longcope C, Stampfer MJ (August 1996). "Prospective study of sex hormone levels and risk of prostate cancer". J. Natl. Cancer Inst. 88 (16): 1118–26. doi:10.1093/jnci/88.16.1118. PMID 8757191.
^ Venkateswaran V, Klotz LH (Aug 2010). "Diet and prostate cancer: mechanisms of action and implications for chemoprevention". Nature Reviews Urology. 7 (8): 442–53. doi:10.1038/nrurol.2010.102. PMID 20647991.
^ Key TJ (2011). "Fruit and vegetables and cancer risk". British Journal of Cancer. 104 (1): 6–11. doi:10.1038/sj.bjc.6606032. PMC 3039795. PMID 21119663.For other common cancers, including colorectal, breast and prostate cancer, epidemiological studies suggest little or no association between total fruit and vegetable consumption and risk.
^ Alexander DD, Mink PJ, Cushing CA, Sceurman B (2010). "A review and meta-analysis of prospective studies of red and processed meat intake and prostate cancer". Nutrition Journal. 9: 50. doi:10.1186/1475-2891-9-50. PMC 2987772. PMID 21044319.
^ "Chemicals in Meat Cooked at High Temperatures and Cancer Risk". National Cancer Institute. 2018-04-02. Archived from the original on 2011-11-06.
^ Wigle DT, Turner MC, Gomes J, Parent ME (March 2008). "Role of hormonal and other factors in human prostate cancer". Journal of Toxicology and Environmental Health. Part B, Critical Reviews. 11 (3–4): 242–59. doi:10.1080/10937400701873548. PMID 18368555.
^ Qin X, Cui Y, Shen L, Sun N, Zhang Y, Li J, et al. (Jan 22, 2013). "Folic acid supplementation and cancer risk: A meta-analysis of randomized controlled trials". International Journal of Cancer. 133 (5): 1033–41. doi:10.1002/ijc.28038. PMID 23338728.
^ Jacobs EJ, Rodriguez C, Mondul AM, Connell CJ, Henley SJ, Calle EE, Thun MJ (July 2005). "A large cohort study of aspirin and other nonsteroidal anti-inflammatory drugs and prostate cancer incidence". J. Natl. Cancer Inst. 97 (13): 975–80. doi:10.1093/jnci/dji173. PMID 15998950.
^ Shannon J, Tewoderos S, Garzotto M, Beer TM, Derenick R, Palma A, Farris PE (August 2005). "Statins and prostate cancer risk: a case-control study". Am. J. Epidemiol. 162 (4): 318–25. doi:10.1093/aje/kwi203. PMID 16014776.
^ Dennis LK, Lynch CF, Torner JC (July 2002). "Epidemiologic association between prostatitis and prostate cancer". Urology. 60 (1): 78–83. doi:10.1016/S0090-4295(02)01637-0. PMID 12100928.
^ Heidegger I, Borena W, Pichler R (May 2015). "The role of human papilloma virus in urological malignancies". Anticancer Research. 35 (5): 2513–9. PMID 25964524.
^ Cai T, Di Vico T, Durante J, Tognarelli A, Bartoletti R (August 2018). "Human Papilloma Virus (HPV) and genitourinary cancers: a narrative review". Minerva Urologica e Nefrologica = the Italian Journal of Urology and Nephrology. 70 (6): 579–587. doi:10.23736/S0393-2249.18.03141-7. PMID 30160386.
^ "Veterans exposed to Agent Orange have higher rates of prostate cancer recurrence". Medical College of Georgia News. May 20, 2007.
[permanent dead link]
^ Rider JR, Wilson KM, Sinnott JA, Kelly RS, Mucci LA, Giovannucci EL (December 2016). "Ejaculation Frequency and Risk of Prostate Cancer: Updated Results with an Additional Decade of Follow-up". European Urology. 70 (6): 974–982. doi:10.1016/j.eururo.2016.03.027. PMC 5040619. PMID 27033442.
^ Aboul-Enein BH, Bernstein J, Ross MW (July 2016). "Evidence for Masturbation and Prostate Cancer Risk: Do We Have a Verdict?". Sexual Medicine Reviews. 4 (3): 229–234. doi:10.1016/j.sxmr.2016.02.006. PMID 27871956.
^ "?". Archived from the original on 27 September 2006. Retrieved 9 August 2010.
^ Aumüller G (1979). Prostate Gland and Seminal Vesicles. Berlin-Heidelberg: Springer-Verlag.
^ Moore KL, Chubb D (1999). Clinically Oriented Anatomy. Baltimore, Maryland: Lippincott Williams & Wilkins. ISBN 978-0-683-06132-1.
^ Steive H (1930). "Männliche Genitalorgane". Handbuch der mikroskopischen Anatomie des Menschen. Vol. VII Part 2. Berlin: Springer. pp. 1–399.
^ "Male Genitals - Prostate Neoplasms". Pathology study images. University of Virginia School of Medicine. Archived from the original on 2011-04-28. Retrieved 2011-04-28.There are many connections between the prostatic venous plexus and the vertebral veins. The veins forming the prostatic plexus do not contain valves and it is thought that straining to urinate causes prostatic venous blood to flow in a reverse direction and enter the vertebral veins carrying malignant cells to the vertebral column.
^ Journal-molecular cancer, review, 2006 5:17, doi:10.1186/1476-4598-5-17
^ "Scientists Discover Anti-Cancer Mechanism that Arrests Early Prostate Cancer". August 4, 2005. Archived from the original on May 19, 2008.
^ Leav I, Plescia J, Goel HL, Li J, Jiang Z, Cohen RJ, Languino LR, Altieri DC (January 2010). "Cytoprotective Mitochondrial Chaperone TRAP-1 As a Novel Molecular Target in Localized and Metastatic Prostate Cancer". Am. J. Pathol. 176 (1): 393–401. doi:10.2353/ajpath.2010.090521. PMC 2797899. PMID 19948822.
^ Zha J, Huang YF (September 2009). "[TGF-beta/Smad in prostate cancer: an update]". Zhonghua Nan Ke Xue (in Chinese). 15 (9): 840–3. PMID 19947572.
^ Watanabe SI, Miyata Y, Kanda S, Iwata T, Hayashi T, Kanetake H, Sakai H (November 2009). "Expression of X-linked inhibitor of apoptosis protein in human prostate cancer specimens with and without neo-adjuvant hormonal therapy". J Cancer Res Clin Oncol. 136 (5): 787–93. doi:10.1007/s00432-009-0718-x. PMID 19946707.
^ Senapati S, Rachagani S, Chaudhary K, Johansson SL, Singh RK, Batra SK (March 2010). "Overexpression of macrophage inhibitory cytokine-1 induces metastasis of human prostate cancer cells through the FAK–RhoA signaling pathway". Oncogene. 29 (9): 1293–302. doi:10.1038/onc.2009.420. PMC 2896817. PMID 19946339.
^ Narizhneva NV, Tararova ND, Ryabokon P, Shyshynova I, Prokvolit A, Komarov PG, et al. (December 2009). "Small molecule screening reveals a transcription-independent pro-survival function of androgen receptor in castration-resistant prostate cancer". Cell Cycle. 8 (24): 4155–67. doi:10.4161/cc.8.24.10316. PMC 2896895. PMID 19946220.
^ Yao V, Berkman CE, Choi JK, O'Keefe DS, Bacich DJ (February 2010). "Expression of prostate-specific membrane antigen (PSMA), increases cell folate uptake and proliferation and suggests a novel role for PSMA in the uptake of the non-polyglutamated folate, folic acid". Prostate. 70 (3): 305–16. doi:10.1002/pros.21065. PMID 19830782.
^ "Cancer Screening Guidelines | Detecting Cancer Early". Archived from the original on 2011-06-13. Retrieved 2011-06-16. American Cancer Society American Cancer Society Guidelines for the early detection of cancer Cited: September 2011
^ Bonekamp D, Jacobs MA, El-Khouli R, Stoianovici D, Macura KJ (May–June 2011). "Advancements in MR Imaging of the Prostate: From Diagnosis to Interventions". Radiographics. 31 (3 Suppl): 677–703. doi:10.1148/rg.313105139. PMC 3093638. PMID 21571651.
^ Barentsz JO, Richenberg J, Clements R, Choyke P, Verma S, Villeirs G, Rouviere O, Logager V, Fütterer JJ (2012). "ESUR prostate MR guidelines 2012". European Radiology. 22 (4): 746–57. doi:10.1007/s00330-011-2377-y. PMC 3297750. PMID 22322308.
^ Natarajan S, Marks LS, Margolis DJ, Huang J, Macairan ML, Lieu P, Fenster A (May 2011). "Clinical application of a 3D ultrasound-guided prostate biopsy system". Urol Oncol. 29 (3 Suppl): 334–42. doi:10.1016/j.urolonc.2011.02.014. PMC 3432280. PMID 21555104.
^ Tan N, Margolis DJ, McClure TD, Thomas A, Finley DS, Reiter RE, Huang J, Raman SS (October 2011). "Radical prostatectomy: value of prostate MRI in surgical planning". Abdominal Imaging. 37 (4): 664–74. doi:10.1007/s00261-011-9805-y. PMID 21993567.
^ Yaghi MD, Kehinde EO (2015). "Oral antibiotics in trans-rectal prostate biopsy and its efficacy to reduce infectious complications: Systematic review". Urology Annals. 7 (4): 417–27. doi:10.4103/0974-7796.164860. PMC 4660689. PMID 26538868.
^ Zani EL, Clark OA, Rodrigues Netto N (May 2011). "Antibiotic prophylaxis for transrectal prostate biopsy". The Cochrane Database of Systematic Reviews (5): CD006576. doi:10.1002/14651858.CD006576.pub2. PMID 21563156.
^ Essink-Bot ML, de Koning HJ, Nijs HG, Kirkels WJ, van der Maas PJ, Schröder FH (June 1998). "Short-term effects of population-based screening for prostate cancer on health-related quality of life". Journal of the National Cancer Institute. 90 (12): 925–31. doi:10.1093/jnci/90.12.925. PMID 9637143.
^ ab Figueiredo JC, Grau MV, Haile RW, Sandler RS, Summers RW, Bresalier RS, Burke CA, McKeown-Eyssen GE, Baron JA (March 2009). "Folic Acid and Risk of Prostate Cancer: Results From a Randomized Clinical Trial". J. Natl. Cancer Inst. 101 (6): 432–5. doi:10.1093/jnci/djp019. PMC 2657096. PMID 19276452.
^ Chuang AY, DeMarzo AM, Veltri RW, Sharma RB, Bieberich CJ, Epstein JI (August 2007). "Immunohistochemical differentiation of high-grade prostate carcinoma from urothelial carcinoma". Am. J. Surg. Pathol. 31 (8): 1246–55. doi:10.1097/PAS.0b013e31802f5d33. PMID 17667550.
^ ab Nutting C, Horwich A, Fisher C, Parsons C, Dearnaley DP (June 1997). "Small-cell carcinoma of the prostate". Journal of the Royal Society of Medicine. 90 (6): 340–1. doi:10.1177/014107689709000615. PMC 1296316. PMID 9227387.
^ ab Wei ZF, Xu H, Wang H, Wei W, Cheng W, Zhou WQ, Ge JP, Zhang ZY, Gao JP, Yin HL (September 2009). "[Clinicopathological characterization of prostatic small cell carcinoma: a case report and review of the literature]". Zhonghua Nan Ke Xue (in Chinese). 15 (9): 829–32. PMID 19947569.
^ Catz SD, Johnson JL (January 2003). "BCL-2 in prostate cancer: a minireview". Apoptosis. 8 (1): 29–37. doi:10.1023/A:1021692801278. PMID 12510149.
^ Chakravarthi S, Thanikachalam P, Nagaraja HS, Yang DL, Bukhari NI (2009). "Assessment of proliferative index and its association with Ki-67 antigen molecule expression in nodular hyperplasia of prostate". Indian Journal of Science & Technology. 2 (8): 1–4.
^ BMJ Group (8 December 2009). "Prostate cancer: How far has your cancer spread? The TNM system". London: Guardian.co.uk. Retrieved 9 August 2010.
^ American Society of Clinical Oncology (2013). "Five things physicians and patients should question" (PDF). The Journal of the Oklahoma State Medical Association. 106 (4): 150–1. PMID 23795527. Archived from the original (PDF) on 2012-07-31.
Makarov DV, Desai RA, Yu JB, Sharma R, Abraham N, Albertsen PC, Penson DF, Gross CP (2012). "The population level prevalence and correlates of appropriate and inappropriate imaging to stage incident prostate cancer in the medicare population". The Journal of Urology. 187 (1): 97–102. doi:10.1016/j.juro.2011.09.042. PMID 22088337.
National Comprehensive Cancer Network - Prostate (2012). "NCCN Clinical Practice Guidelines in Oncology". nccn.org. Archived from the original on 9 November 2012. Retrieved 15 November 2012.
Thompson I, Thrasher JB, Aus G, Burnett AL, Canby-Hagino ED, Cookson MS, et al. (2007). "Guideline for the management of clinically localized prostate cancer: 2007 update". The Journal of Urology. 177 (6): 2106–31. doi:10.1016/j.juro.2007.03.003. PMID 17509297.
^ abcde Masko EM, Allott EH, Freedland SJ (May 2013). "The relationship between nutrition and prostate cancer: is more always better?". European Urology. 63 (5): 810–20. doi:10.1016/j.eururo.2012.11.012. PMC 3597758. PMID 23219353.
^ Thompson AK, Shaw DI, Minihane AM, Williams CM (December 2008). "Trans-fatty acids and cancer: the evidence reviewed". Nutrition Research Reviews. 21 (2): 174–88. doi:10.1017/S0954422408110964. PMID 19087370.
^ Heinze VM, Actis AB (February 2012). "Dietary conjugated linoleic acid and long-chain n-3 fatty acids in mammary and prostate cancer protection: a review". International Journal of Food Sciences and Nutrition. 63 (1): 66–78. doi:10.3109/09637486.2011.598849. PMID 21762028.
^ Datta M, Schwartz GG (2012). "Calcium and vitamin D supplementation during androgen deprivation therapy for prostate cancer: a critical review". The Oncologist. 17 (9): 1171–9. doi:10.1634/theoncologist.2012-0051. PMC 3448410. PMID 22836449.
^ Szymanski KM, Wheeler DC, Mucci LA (November 2010). "Fish consumption and prostate cancer risk: a review and meta-analysis". The American Journal of Clinical Nutrition. 92 (5): 1223–33. doi:10.3945/ajcn.2010.29530. PMID 20844069.
^ American Dietetic Association and Dieticians of Canada (June 2003). "Position of the American Dietetic Association and Dietitians of Canada: Vegetarian diets". Journal of the American Dietetic Association. 103 (6): 748–65. doi:10.1053/jada.2003.50142. PMID 12778049.
^ World Cancer Research Fund; American Institute for Cancer (2007). Food, nutrition, physical activity, and the prevention of cancer a global perspective (PDF). Washington, D.C.: American Institute for Cancer Research. p. 76. ISBN 978-0-9722522-2-5. Archived from the original (PDF) on 2013-05-23.
^ Rowles JL, Ranard KM, Applegate CC, Jeon S, An R, Erdman JW (September 2018). "Processed and raw tomato consumption and risk of prostate cancer: a systematic review and dose-response meta-analysis". Prostate Cancer and Prostatic Diseases. 21 (3): 319–336. doi:10.1038/s41391-017-0005-x. PMID 29317772.
^ ab "American Cancer Society Guidelines on Nutrition and Physical Activity for Cancer Prevention" (PDF). Last Revised: 1/11/2012. Archived (PDF) from the original on 2012-06-25.
^ Wilt TJ, MacDonald R, Hagerty K, Schellhammer P, Kramer BS (2008). Wilt TJ, ed. "Five-alpha-reductase Inhibitors for prostate cancer prevention". Cochrane Database Syst Rev (2): CD007091. doi:10.1002/14651858.CD007091. PMID 18425978.
^ ab Alberts AR, Schoots IG, Roobol MJ (June 2015). "Prostate-specific antigen-based prostate cancer screening: Past and future". International Journal of Urology. 22 (6): 524–32. doi:10.1111/iju.12750. PMID 25847604.
^ ab Rendon RA, Mason RJ, Marzouk K, Finelli A, Saad F, So A, Violette P, Breau RH (October 2017). "Canadian Urological Association recommendations on prostate cancer screening and early diagnosis". Canadian Urological Association Journal. 11 (10): 298–309. doi:10.5489/cuaj.4888. PMC 5659858. PMID 29381452.
^ "Home Page - USPSTF Draft Prostate Screening Recommendations". USPSTF Draft Prostate Screening Recommendations. Retrieved 2 March 2018.
^ Mulhem E, Fulbright N, Duncan N (October 2015). "Prostate Cancer Screening". American Family Physician. 92 (8): 683–8. PMID 26554408.
^ Prostate Cancer Screening Archived 2017-09-07 at the Wayback Machine CDC, updated April 6, 2010
^ Qaseem A, Barry MJ, Denberg TD, Owens DK, Shekelle P (May 2013). "Screening for prostate cancer: a guidance statement from the Clinical Guidelines Committee of the American College of Physicians". Annals of Internal Medicine. 158 (10): 761–769. doi:10.7326/0003-4819-158-10-201305210-00633. PMID 23567643.
^ Basch E, Oliver TK, Vickers A, Thompson I, Kantoff P, Parnes H, Loblaw DA, Roth B, Williams J, Nam RK (August 2012). "Screening for prostate cancer with prostate-specific antigen testing: American Society of Clinical Oncology Provisional Clinical Opinion". Journal of Clinical Oncology. 30 (24): 3020–5. doi:10.1200/JCO.2012.43.3441. PMC 3776923. PMID 22802323.
^ "EARLY DETECTION OF PROSTATE CANCER: AUA GUIDELINE". American Urological Association. 2013. Archived from the original on 7 May 2013. Retrieved 10 May 2013.
^ abcd Filson CP, Marks LS, Litwin MS (8 May 2015). "Expectant management for men with early stage prostate cancer". Ca. 65 (4): 265–82. doi:10.3322/caac.21278. PMID 25958817.
^ Lu-Yao GL, Albertsen PC, Moore DF, Shih W, Lin Y, DiPaola RS, et al. (September 2009). "Outcomes of Localized Prostate Cancer Following Conservative Management". The Journal of the American Medical Association. 302 (11): 1202–09. doi:10.1001/jama.2009.1348. PMC 2822438. PMID 19755699.
^ Mongiat-Artus P, Peyromaure M, Richaud P, Droz JP, Rainfray M, Jeandel C, et al. (December 2009). "[Recommendations for the treatment of prostate cancer in the elderly man: A study by the oncology committee of the French association of urology]". Prog. Urol. (in French). 19 (11): 810–7. doi:10.1016/j.purol.2009.02.008. PMID 19945664.
^ Picard JC, Golshayan AR, Marshall DT, Opfermann KJ, Keane TE (November 2009). "The multi-disciplinary management of high-risk prostate cancer". Urol. Oncol. 30 (1): 3–15. doi:10.1016/j.urolonc.2009.09.002. PMID 19945310.
^ ab Mohan R, Schellhammer PF (August 2011). "Treatment options for localized prostate cancer". American Family Physician. 84 (4): 413–20. PMID 21842788.
^ Wallis CJ, Glaser A, Hu JC, Huland H, Lawrentschuk N, Moon D, Murphy DG, Nguyen PL, Resnick MJ, Nam RK (January 2018). "Survival and Complications Following Surgery and Radiation for Localized Prostate Cancer: An International Collaborative Review". European Urology. 73 (1): 11–20. doi:10.1016/j.eururo.2017.05.055. PMID 28610779.
^ Chen C, Chen Z, Wang K, Hu L, Xu R, He X (November 2017). "Comparisons of health-related quality of life among surgery and radiotherapy for localized prostate cancer: a systematic review and meta-analysis". Oncotarget. 8 (58): 99057–99065. doi:10.18632/oncotarget.21519. PMC 5716791. PMID 29228751.
^ Mouraviev V, Evans B, Polascik TJ (2006). "Salvage prostate cryoablation after primary interstitial brachytherapy failure: a feasible approach". Prostate Cancer and Prostatic Diseases. 9 (1): 99–101. doi:10.1038/sj.pcan.4500853. PMID 16314889.
^ Wallis CJ, Mahar AL, Choo R, Herschorn S, Kodama RT, Shah PS, Danjoux C, Narod SA, Nam RK (March 2016). "Second malignancies after radiotherapy for prostate cancer: systematic review and meta-analysis". BMJ. 352: i851. doi:10.1136/bmj.i851. PMC 4775870. PMID 26936410.
^ Hegarty J, Beirne PV, Walsh E, Comber H, Fitzgerald T, Wallace Kazer M (Nov 10, 2010). Hegarty J, ed. "Radical prostatectomy versus watchful waiting for prostate cancer". Cochrane Database of Systematic Reviews (11): CD006590. doi:10.1002/14651858.CD006590.pub2. PMID 21069689.
^ de Jong Y, Pinckaers JH, ten Brinck RM, Lycklama à Nijeholt AA, Dekkers OM (2014). "Urinating standing versus sitting: position is of influence in men with prostate enlargement. A systematic review and meta-analysis". PLOS One. 9 (7): e101320. Bibcode:2014PLoSO...9j1320D. doi:10.1371/journal.pone.0101320. PMC 4106761. PMID 25051345.
^ "Active Surveillance May Be Preferred Option in Some Men with Prostate Cancer". Cancer.gov. 2011-04-19. Archived from the original on 2011-05-03. Retrieved 2011-08-29.
^ ab Sartor O, de Bono JS (February 2018). "Metastatic Prostate Cancer". The New England Journal of Medicine. 378 (7): 645–657. doi:10.1056/NEJMra1701695. PMID 29412780.
^ ab Hong H, Zhang Y, Sun J, Cai W (June 2010). "Positron emission tomography imaging of prostate cancer". Amino Acids. 39 (1): 11–27. doi:10.1007/s00726-009-0394-9. PMC 2883014. PMID 19946787.
^ ab Peyromaure M, Valéri A, Rebillard X, Beuzeboc P, Richaud P, Soulié M, Salomon L (December 2009). "[Characteristics of prostate cancer in men less than 50-year-old]". Progres en Urologie (in French). 19 (11): 803–9. doi:10.1016/j.purol.2009.04.010. PMID 19945663.
^ Fitzpatrick JM (2008). "Management of localized prostate cancer in senior adults: the crucial role of comorbidity". BJU International. 101 Suppl 2: 16–22. doi:10.1111/j.1464-410X.2007.07487.x. PMID 18307688.
^ "Evidence-Based Cancer Guidelines, Oncology Drug Compendium, Oncology Continuing Medical Education". NCCN. Retrieved 2011-08-29.
^ Dhondt B, De Bleser E, Claeys T, Buelens S, Lumen N, Vandesompele J, et al. (December 2018). "Discovery and validation of a serum microRNA signature to characterize oligo- and polymetastatic prostate cancer: not ready for prime time". World Journal of Urology. doi:10.1007/s00345-018-2609-8. PMID 30578441.
^ Hammerstrom AE, Cauley DH, Atkinson BJ, Sharma P (August 2011). "Cancer immunotherapy: sipuleucel-T and beyond". Pharmacotherapy. 31 (8): 813–28. doi:10.1592/phco.31.8.813. PMC 4159742. PMID 21923608.
^ Seruga B, Ocana A, Tannock IF (January 2011). "Drug resistance in metastatic castration-resistant prostate cancer". Nature Reviews Clinical Oncology. 8 (1): 12–23. doi:10.1038/nrclinonc.2010.136. PMID 20859283.
^ Clarke NW (c. 2005). "Docetaxel for the Treatment of Hormone Refractory Prostate Cancer" (PDF). Archived from the original (PDF) on 2012-07-12.
^ "Prostate cancer (hormone-refractory) - docetaxel". National Institute for Health and Clinical Excellence. 2010-12-10. Archived from the original on 2012-02-02. Retrieved 2011-07-04.
^ de Bono JS, Oudard S, Ozguroglu M, Hansen S, Machiels JP, Kocak I, Gravis G, Bodrogi I, Mackenzie MJ, Shen L, Roessner M, Gupta S, Sartor AO (October 2010). "Prednisone plus cabazitaxel or mitoxantrone for metastatic castration-resistant prostate cancer progressing after docetaxel treatment: a randomised open-label trial". Lancet. 376 (9747): 1147–54. doi:10.1016/S0140-6736(10)61389-X. PMID 20888992.
^ "Avastin, Thalomid, Taxotere, and Prednisone Effective for Men with Hormone Refractory Prostate Cancer". March 2010. Archived from the original on 15 June 2010. Retrieved 10 May 2010.
^ Kantoff PW, Higano CS, Shore ND, Berger ER, Small EJ, Penson DF, Redfern CH, Ferrari AC, Dreicer R, Sims RB, Xu Y, Frohlich MW, Schellhammer PF (July 2010). "Sipuleucel-T immunotherapy for castration-resistant prostate cancer". N. Engl. J. Med. 363 (5): 411–22. doi:10.1056/NEJMoa1001294. PMID 20818862.
^ "FDA approves Zytiga for late-stage prostate cancer". U.S. Food and Drug Administration. 2011-04-28. Archived from the original on 2013-09-22.
^ ab "FDA approves new treatment for a type of late stage prostate cancer". press release. United States Food and Drug Administration. 2012-08-31. Archived from the original on 2013-10-02.
^ ab Anna Azvolinsky (September 4, 2012). "FDA Approves Enzalutamide (Xtandi) for Late-Stage Prostate Cancer". CancerNetwork. Archived from the original on September 13, 2012.
^ Qin J, Liu X, Laffin B, Chen X, Choy G, Jeter CR, et al. (2012). "The PSA−/lo Prostate Cancer Cell Population Harbors Self-Renewing Long-Term Tumor-Propagating Cells that Resist Castration". Cell Stem Cell. 10 (5): 556–69. doi:10.1016/j.stem.2012.03.009. PMC 3348510. PMID 22560078.
^ Maitland NJ, Collins AT (2008). "Prostate cancer stem cells—a new target for therapy". Journal of Clinical Oncology. 26 (17): 2862–70. doi:10.1200/JCO.2007.15.1472. PMID 18539965.
^ Attard G, Richards J, de Bono JS (2011). "New strategies in metastatic prostate cancer: targeting the androgen receptor signaling pathway". Clinical Cancer Research. 17 (7): 1649–57. doi:10.1158/1078-0432.CCR-10-0567. PMC 3513706. PMID 21372223. Archived from the original on 2011-08-04.
^ Rane JK, Pellacani D, Maitland NJ (2012). "Advanced prostate cancer—a case for adjuvant differentiation therapy". Nature Reviews Urology. 9 (10): 595–602. doi:10.1038/nrurol.2012.157. PMID 22890299.
^ "Cancer of the Prostate - Cancer Stat Facts". seer.cancer.gov. Archived from the original on 18 March 2017. Retrieved 11 April 2017.
^ Wakai K (February 2005). "[Descriptive epidemiology of prostate cancer in Japan and Western countries]". Nippon Rinsho (in Japanese). 63 (2): 207–12. PMID 15714967.
^ Jaubert de Beaujeu M, Chavrier Y (January 1976). "[Deformations of the anterior thoracic wall (author's transl)]". Ann Chir Thorac Cardiovasc (in French). 15 (1): 1–6. PMID 1259345.
^ Hsing AW, Tsao L, Devesa SS (January 2000). "International trends and patterns of prostate cancer incidence and mortality". Int. J. Cancer. 85 (1): 60–7. doi:10.1002/(SICI)1097-0215(20000101)85:1<60::AID-IJC11>3.0.CO;2-B. PMID 10585584.
^ Osegbe DN (April 1997). "Prostate cancer in Nigerians: facts and nonfacts". J. Urol. 157 (4): 1340–3. doi:10.1016/S0022-5347(01)64966-8. PMID 9120935.
^ Bello JO (May 2017). "Predictors of survival outcomes in native sub Saharan black men newly diagnosed with metastatic prostate cancer". BMC Urology. 17 (1): 39. doi:10.1186/s12894-017-0228-0. PMC 5450414. PMID 28558685.
^ Di Blasio CJ, Rhee AC, Cho D, Scardino PT, Kattan MW (October 2003). "Predicting clinical end points: treatment nomograms in prostate cancer". Semin. Oncol. 30 (5): 567–86. doi:10.1016/S0093-7754(03)00351-8. PMID 14571407.
^ Huggins C, Steven RE, Hodges CV (1941). "Studies on prostatic cancer". Arch. Surg. 43 (2): 209–223. doi:10.1001/archsurg.1941.01210140043004.
^ Hellerstedt BA, Pienta KJ (2002). "The current state of hormonal therapy for prostate cancer". CA Cancer J Clin. 52 (3): 154–79. doi:10.3322/canjclin.52.3.154. PMID 12018929.
^ Feldman BJ, Feldman D (October 2001). "The development of androgen-independent prostate cancer". Nature Reviews Cancer. 1 (1): 34–45. doi:10.1038/35094009. PMID 11900250.
^ Eifler J. B.; Feng Z.; Lin B. M.; Partin M. T.; Humphreys E. B.; Han M.; Epstein J. I.; Walsh P. C.; Trock B. J.; et al. (2013). "An updated prostate cancer staging nomogram (Partin tables) based on cases from 2006 to 2011". BJU International. 111 (1): 22–29. doi:10.1111/j.1464-410X.2012.11324.x. PMC 3876476. PMID 22834909.
^ Cooperberg MR, Pasta DJ, Elkin EP, Litwin MS, Latini DM, Du Chane J, et al. (June 2005). "The UCSF Cancer of the Prostate Risk Assessment (CAPRA) Score: a straightforward and reliable preoperative predictor of disease recurrence after radical prostatectomy". J. Urol. 173 (6): 1938–42. doi:10.1097/01.ju.0000158155.33890.e7. PMC 2948569. PMID 15879786.
^ Cooperberg MR, Freedland SJ, Pasta DJ, Elkin EP, Presti JC, Amling CL, et al. (November 2006). "Multiinstitutional validation of the UCSF cancer of the prostate risk assessment for prediction of recurrence after radical prostatectomy". Cancer. 107 (10): 2384–91. doi:10.1002/cncr.22262. PMID 17039503.
^ May M, Knoll N, Siegsmund M, Fahlenkamp D, Vogler H, Hoschke B, Gralla O (November 2007). "Validity of the CAPRA score to predict biochemical recurrence-free survival after radical prostatectomy. Results from a European multicenter survey of 1,296 patients". J. Urol. 178 (5): 1957–62, discussion 1962. doi:10.1016/j.juro.2007.07.043. PMID 17868719.
^ Zhao KH, Hernandez DJ, Han M, Humphreys EB, Mangold LA, Partin AW (August 2008). "External validation of University of California, San Francisco, Cancer of the Prostate Risk Assessment score". Urology. 72 (2): 396–400. doi:10.1016/j.urology.2007.11.165. PMID 18372031.
^ Cooperberg MR, Broering JM, Carroll PR (June 2009). "Risk Assessment for Prostate Cancer Metastasis and Mortality at the Time of Diagnosis". J. Natl. Cancer Inst. 101 (12): 878–87. doi:10.1093/jnci/djp122. PMC 2697208. PMID 19509351.
^ "CDC FastStats". Centers for Disease Control. Archived from the original on 2017-07-28.
^ "Treatment Choices for Men With Early-Stage Prostate Cancer". National Cancer Institute. 2014-10-17. Archived from the original on 2015-04-04.
^ Eggener SE, Badani K, Barocas DA, Barrisford GW, Cheng JS, Chin AI, Corcoran A, Epstein JI, George AK, Gupta GN, Hayn MH, Kauffman EC, Lane B, Liss MA, Mirza M, Morgan TM, Moses K, Nepple KG, Preston MA, Rais-Bahrami S, Resnick MJ, Siddiqui MM, Silberstein J, Singer EA, Sonn GA, Sprenkle P, Stratton KL, Taylor J, Tomaszewski J, Tollefson M, Vickers A, White WM, Lowrance WT (Apr 2015). "Gleason 6 Prostate Cancer: Translating Biology into Population Health". J Urol. 194 (3): 626–634. doi:10.1016/j.juro.2015.01.126. PMC 4551510. PMID 25849602.CS1 maint: Multiple names: authors list (link)
^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 2009-11-11. Retrieved Nov 11, 2009.
^ World Cancer Report 2014. International Agency for Research on Cancer, World Health Organization. 2014. ISBN 978-92-832-0432-9.
^ Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011). "Global cancer statistics". CA – A Cancer Journal for Clinicians. 61 (2): 69–90. doi:10.3322/caac.20107. PMID 21296855.
^ Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, Adair T, Aggarwal R, Ahn SY, et al. (Dec 15, 2012). "Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet. 380 (9859): 2095–128. doi:10.1016/S0140-6736(12)61728-0. PMID 23245604.
^ "Prostate Cancer Statistics". Laparoscopic Urology. Archived from the original on 24 June 2016. Retrieved 19 June 2016.
^ ab Overview: Prostate Cancer—What Causes Prostate Cancer? Archived 2006-04-04 at the Wayback Machine American Cancer Society (2 May 2006). Retrieved on 5 April 2007
^ ab Prostate Cancer FAQs. Archived 2006-05-29 at the Wayback Machine State University of New York School of Medicine Department of Urology (31 August 2006). Retrieved on 5 April 2007
^ Lee MM, Gomez SL, Chang JS, Wey M, Wang RT, Hsing AW (Jul 2003). "Soy and isoflavone consumption in relation to prostate cancer risk in China". Cancer Epidemiol Biomarkers Prev. 12 (7): 665–8. PMID 12869409.
^ Potosky AL, Miller BA, Albertsen PC, Kramer BS (February 1995). "The role of increasing detection in the rising incidence of prostate cancer". JAMA. 273 (7): 548–52. doi:10.1001/jama.273.7.548. PMID 7530782.
^ Hanno P.M., Malcowicz S. B., Wein A. J., "Clinical Manual of Urology" McGraw Hill 2001
^ Homma Y, Kawabe K, Tsukamoto T, Yamanaka H, Okada K, Okajima E, Yoshida O, Kumazawa J, Gu FL, Lee C, Hsu TC, dela Cruz RC, Tantiwang A, Lim PH, Sheikh MA, Bapat SD, Marshall VR, Tajima K, Aso Y (1997). "Epidemiologic survey of lower urinary tract symptoms in Asia and Australia using the international prostate symptom score". International Journal of Urology. 4 (1): 40–46. doi:10.1111/j.1442-2042.1997.tb00138.x. PMID 9179665.
^ Bostwick DG, Eble JN (2007). Urological Surgical Pathology. St. Louis: Mosby. p. 468. ISBN 978-0-323-01970-5.
^ Woloshin, Steve; Schwartz, Lisa A. (2011). Overdiagnosed: Making People Sick in the Pursuit of Health. USA: Beacon Press. pp. 45–60. ISBN 978-0-8070-2200-9.
^ PDQ Screening and Prevention Editorial Board (2002). "Prostate Cancer Screening (PDQ®): Health Professional Version". PDQ Cancer Information Summaries. Bethesda (MD): National Cancer Institute (US). PMID 26389383. This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
^ Ferlay J, Steliarova-Foucher E, Lortet-Tieulent J, Rosso S, Coebergh JW, Comber H, Forman D, Bray F (April 2013). "Cancer incidence and mortality patterns in Europe: estimates for 40 countries in 2012". European Journal of Cancer. 49 (6): 1374–403. doi:10.1016/j.ejca.2012.12.027. PMID 23485231.
^ "Prostate cancer statistics". Cancer Research UK. Archived from the original on 6 October 2014. Retrieved 3 October 2014.
^ Adams J (1853). "The case of scirrhous of the prostate gland with corresponding affliction of the lymphatic glands in the lumbar region and in the pelvis". Lancet. 1 (1547): 393–394. doi:10.1016/S0140-6736(02)68759-8.
^ Lytton B (June 2001). "Prostate cancer: a brief history and the discovery of hormonal ablation treatment". The Journal of Urology. 165 (6 Pt 1): 1859–62. doi:10.1016/S0022-5347(05)66228-3. PMID 11371867.
^ Young HH (1905). "Four cases of radical prostatectomy". Johns Hopkins Bull. 16.
^ Walsh PC, Lepor H, Eggleston JC (1983). "Radical prostatectomy with preservation of sexual function: anatomical and pathological considerations". The Prostate. 4 (5): 473–85. doi:10.1002/pros.2990040506. PMID 6889192.
^ Huggins CB, Hodges CV (1941). "Studies on prostate cancer: 1. The effects of castration, of estrogen and androgen injection on serum phosphatases in metastatic carcinoma of the prostate". Cancer Res. 1 (4): 293. Archived from the original on 2017-06-30.
^ Schally AV, Kastin AJ, Arimura A (November 1971). "Hypothalamic follicle-stimulating hormone (FSH) and luteinizing hormone (LH)-regulating hormone: structure, physiology, and clinical studies". Fertility and Sterility. 22 (11): 703–21. doi:10.1016/S0015-0282(16)38580-6. PMID 4941683.
^ Tolis G, Ackman D, Stellos A, Mehta A, Labrie F, Fazekas AT, Comaru-Schally AM, Schally AV (March 1982). "Tumor growth inhibition in patients with prostatic carcinoma treated with luteinizing hormone-releasing hormone agonists". Proc. Natl. Acad. Sci. U.S.A. 79 (5): 1658–62. Bibcode:1982PNAS...79.1658T. doi:10.1073/pnas.79.5.1658. PMC 346035. PMID 6461861.
^ Denmeade SR, Isaacs JT (May 2002). "A history of prostate cancer treatment". Nature Reviews Cancer. 2 (5): 389–96. doi:10.1038/nrc801. PMC 4124639. PMID 12044015.
^ Scott WW, Johnson DE, Schmidt JE, Gibbons RP, Prout GR, Joiner JR, Saroff J, Murphy GP (December 1975). "Chemotherapy of advanced prostatic carcinoma with cyclophosphamide or 5-fluorouracil: results of first national randomized study". The Journal of Urology. 114 (6): 909–11. doi:10.1016/S0022-5347(17)67172-6. PMID 1104900.
^ abc Arnst C (2007-06-13). "A Gender Gap in Cancer". Businessweek.com. Archived from the original on 2011-08-06. Retrieved 2011-08-29.
^ Browne A (2001-10-07). "Cancer bias puts breasts first". The Guardian. London. Archived from the original on 2016-12-26.
^ Templeton S (2005-10-16). "Men lose out in battle for cancer cash". Sunday Times. Archived from the original on 2011-05-24.
^ Farrell W, Sterba JP (2008-07-24). Does feminism discriminate against ... - Google Books. ISBN 978-0-19-531283-6. Retrieved 2011-08-29.
^ National Prostate Cancer Coalition. The Prostate Cancer Gap. A Crisis in Men’s Health. National Prostate Cancer Coalition; 2007 Webcite
^ "Breast cancer receives much more research funding, publicity than prostate cancer despite similar number of victims". The Daily Caller. 2010-10-05. Archived from the original on 2011-10-13. Retrieved 2011-08-29.
^ "Prostate cancer in shadow of female counterpart". MSNBC. 2005-03-28. Archived from the original on 2012-11-24. Retrieved 2011-08-29.
^ "Archived copy". Archived from the original on 2011-07-21. Retrieved 2010-11-04.CS1 maint: Archived copy as title (link) ClinicalTrials.gov listing of MDV3100 articles
^ "Positive Outcome of Interim Analysis of pivotal Alpharadin study: Primary endpoint met in Phase III ALSYMPCA study". Press Release. Algeta.com. 2011-06-06. Archived from the original on 2011-08-11. Retrieved 2011-07-04.
^ "FDA approves new drug for advanced prostate cancer" (Press release). Food and Drug Administration. 15 May 2013. Archived from the original on 4 June 2013.
^ ab Geethakumari PR, Cookson MS, Kelly WK (15 February 2016). "The Evolving Biology of Castration-Resistant Prostate Cancer: Review of Recommendations From the Prostate Cancer Clinical Trials Working Group 3". Oncology. 30 (2): 187–195, 199. Archived from the original on 22 February 2016.
^ abcd Elshan ND, Rettig MB, Jung ME (22 November 2018). "Molecules targeting the androgen receptor (AR) signaling axis beyond the AR-Ligand binding domain". Medicinal Research Reviews. 39 (1). doi:10.1002/med.21548. PMID 30565725.
^ abc Ghosh J, Myers CE (October 1998). "Inhibition of arachidonate 5-lipoxygenase triggers massive apoptosis in human prostate cancer cells". Proc. Natl. Acad. Sci. U.S.A. 95 (22): 13182–13187. Bibcode:1998PNAS...9513182G. doi:10.1073/pnas.95.22.13182. PMC 23752. PMID 9789062.Inhibition of 5-lipoxygenase by MK886 completely blocks 5-HETE production and induces massive apoptosis in both hormone-responsive (LNCaP) and -nonresponsive (PC3) human prostate cancer cells. This cell death is very rapid
^ abc Greene ER, Huang S, Serhan CN, Panigrahy D (November 2011). "Regulation of inflammation in cancer by eicosanoids". Prostaglandins Other Lipid Mediat. 96 (1–4): 27–36. doi:10.1016/j.prostaglandins.2011.08.004. PMC 4051344. PMID 21864702.The 5-lipoxygenase (5-LOX) pathway is implicated in the development and progression of human cancers. 5-LOX, whose crystal structure was recently identified (118), is a key enzyme in metabolizing arachidonic acid to leukotrienes. 5-LOX can be induced by pro-inflammatory stimuli and is expressed in epithelial cancers including lung, prostate, breast, and colon (113). Hence, 5-LOX inhibitors have been targeted for their chemopreventive effects. Inhibition of 5-LOX activity is shown to block prostate cancer cell proliferation as well as carcinogen-induced lung tumorigenesis (119, 120). ... Both 5-HETE and 12-HETE are also products of lipoxygenase and are involved in tumor progression (12). Exogenous 5-HETE can stimulate the proliferation of prostate cancer cells and act as a survival factor (137, 138). These results require relatively high concentrations (at a concentration of 10 μM). Blocking the formation of 5-HETE, by inhibiting 5-lipoxygenase, results in massive apoptosis of human prostate cancer cells (139).
^ abc Bishayee K, Khuda-Bukhsh AR (September 2013). "5-lipoxygenase antagonist therapy: a new approach towards targeted cancer chemotherapy". Acta Biochim. Biophys. Sin. (Shanghai). 45 (9): 709–719. doi:10.1093/abbs/gmt064. PMID 23752617.Recent studies demonstrated the involvement of growth factors, such as epidermal growth factor (EGF) and neurotensin in the 5-LOX-mediated tumor progression in prostate cancer [22,23]. Recent studies with 5-LOX siRNA [10] and specific blocker of 5-LOX [24] revealed the relation of this gene with the tumor cell proliferation. ... Meclofenamate sodium (MS) is known for its anti-inflammatory activity, and apart from this, Boctor et al. [37] reported that it caused reduction in the formation of 5-HETE in human leucocytes when used. MS can thus be considered a dual inhibitor of 5-LOX and COX pathways of arachidonic acid cascade. Further investigation with this substance revealed that it could interfere with the LT receptors in the lung carcinoma [38]. In a recent study, a group of scientists have shown the effect of MS on prostate cancer cells both in vitro and in vivo [39], and their result suggests a profound reduction in the tumor growth and cancer metastasis. ... While the commonly used inhibitors produced strong cytotoxicity, notably, zileuton, the only commercialized 5-LOX inhibitor, failed to induce an anti-proliferative or cytotoxic response in all other types of tumor cells where 5-LOX was in inactive state (e.g. HeLa cells). But where 5-LOX was in active state, zileuton could effectively inhibit progression, as in case of prostate cancer.
^ Linja MJ, Savinainen KJ, Saramäki OR, Tammela TL, Vessella RL, Visakorpi T (May 2001). "Amplification and overexpression of androgen receptor gene in hormone-refractory prostate cancer". Cancer Research. 61 (9): 3550–5. PMID 11325816.
^ Ford OH, Gregory CW, Kim D, Smitherman AB, Mohler JL (November 2003). "Androgen receptor gene amplification and protein expression in recurrent prostate cancer". The Journal of Urology. 170 (5): 1817–21. doi:10.1097/01.ju.0000091873.09677.f4. PMID 14532783.
^ Kokontis J, Takakura K, Hay N, Liao S (March 1994). "Increased androgen receptor activity and altered c-myc expression in prostate cancer cells after long-term androgen deprivation". Cancer Research. 54 (6): 1566–73. PMID 7511045.
^ Umekita Y, Hiipakka RA, Kokontis JM, Liao S (October 1996). "Human prostate tumor growth in athymic mice: inhibition by androgens and stimulation by finasteride". Proc. Natl. Acad. Sci. U.S.A. 93 (21): 11802–7. Bibcode:1996PNAS...9311802U. doi:10.1073/pnas.93.21.11802. PMC 38139. PMID 8876218.
^ Kokontis JM, Hsu S, Chuu CP, Dang M, Fukuchi J, Hiipakka RA, Liao S (December 2005). "Role of androgen receptor in the progression of human prostate tumor cells to androgen independence and insensitivity". The Prostate. 65 (4): 287–98. doi:10.1002/pros.20285. PMID 16015608.
^ Urisman A, Molinaro RJ, Fischer N, Plummer SJ, Casey G, Klein EA, Malathi K, Magi-Galluzzi C, Tubbs RR, Ganem D, Silverman RH, DeRisi JL (March 2006). "Identification of a Novel Gammaretrovirus in Prostate Tumors of Patients Homozygous for R462Q RNASEL Variant". PLoS Pathog. 2 (3): e25. doi:10.1371/journal.ppat.0020025. PMC 1434790. PMID 16609730.
^ Schlaberg R, Choe DJ, Brown KR, Thaker HM, Singh IR (September 2009). "XMRV is present in malignant prostatic epithelium and is associated with prostate cancer, especially high-grade tumors". Proc. Natl. Acad. Sci. U.S.A. 106 (38): 16351–6. Bibcode:2009PNAS..10616351S. doi:10.1073/pnas.0906922106. PMC 2739868. PMID 19805305.
^ Hohn O, Krause H, Barbarotto P, Niederstadt L, Beimforde N, Denner J, Miller K, Kurth R, Bannert N (2009). "Lack of evidence for xenotropic murine leukemia virus-related virus (XMRV) in German prostate cancer patients". Retrovirology. 6: 92. doi:10.1186/1742-4690-6-92. PMC 2770519. PMID 19835577.
^ Lee D, Das Gupta J, Gaughan C, Steffen I, Tang N, Luk KC, et al. (2012). Tachedjian G, ed. "In-Depth Investigation of Archival and Prospectively Collected Samples Reveals No Evidence for XMRV Infection in Prostate Cancer". PLOS One. 7 (9): e44954. Bibcode:2012PLoSO...744954L. doi:10.1371/journal.pone.0044954. PMC 3445615. PMID 23028701.
^ Alberts B (Dec 23, 2011). "Retraction". Science. 334 (6063): 1636. Bibcode:2011Sci...334.1636A. doi:10.1126/science.334.6063.1636-a. PMID 22194552.
^ Ross, Susan, ed. (September 2012). "Retraction. Identification of a novel gammaretrovirus in prostate tumors of patients homozygous for R462Q RNASEL variant". PLoS Pathogens. 8 (9): 10.1371/annotation/7e2efc01–2e9b–4e9b–aef0–87ab0e4e4732. doi:10.1371/annotation/7e2efc01-2e9b-4e9b-aef0-87ab0e4e4732. PMC 3445601. PMID 23028303.
^ Bourdoumis A, Papatsoris AG, Chrisofos M, Efstathiou E, Skolarikos A, Deliveliotis C (2010). "The novel prostate cancer antigen 3 (PCA3) biomarker". Int Braz J Urol. 36 (6): 665–8, discussion 669. doi:10.1590/S1677-55382010000600003. PMID 21176272.
External links
| Classification | D
|
|---|---|
| External resources |
|
Prostate cancer at Curlie- Patient-centered information from the European Urological Association